Aesthetic Medicine for the ND
Treatment of Skin Lesions
John Hahn, DPM, ND
As NDs, we always look for ways to help our patients treat skin lesions and avoid surgery whenever possible. Unfortunately, patients may present with various skin lesions that are physically unattractive and could be precancerous. As naturopathic family practitioners, we must sometimes refer these patients with skin lesions to a dermatologist for evaluation and treatment. However, skin lesions that would be amenable to treatment with a shave biopsy or liquid nitrogen can now be treated with a new handheld delivery system for cryosurgery or with high-frequency low-temperature radiowave ablation using a new radiosurgical device.
Cryosurgery and High-Frequency Low-Temperature Radiowave Ablation
Cryosurgery is broadly defined as the controlled destruction of unwanted tissue by precise application of extreme cold in a clinical procedure. It is a well-proven method and may be used to effect selected destruction of living tissue because normal and diseased cellular elements will not survive after being subjected to freezing (−27°C). In cryosurgery, the rate of removal of heat from the tissue is more important than simply the application of extremely low temperatures. Slow heat reduction causes a protective reaction of osmotic fluids flowing out of the cell, leading to cell preservation instead of necrosis. Effective treatment requires rapid freezing of the tissue. From an aesthetic point of view, the physician needs to precisely judge the depth of the freeze to avoid the formation of scar tissue as much as possible. A nitrous oxide–powered handheld cryosurgical instrument (CryoProbe; H&O Equipments NV) will give you a precise depth of penetration at a rate of 1.0 mm per 5 seconds of freeze, and the diameter can be restricted to 0.5 mm.
In my aesthetic practice as an ND, I see many types of skin lesions on physical examination that are amenable to treatment. Removal may prevent some lesions from becoming cancerous in the future. Depending on the location and the type of aesthetic result I am looking for, I treat these patients with cryosurgery or with high-frequency low-temperature radiowave ablation. The aim in using these types of aesthetic surgical instruments is to effect minimal formation of scar tissue. In patients who have skin phototype III, IV, or V on the Fitzpatrick Scale, I often initially treat them with 4% hydroxy for 7 to 10 days on each lesion and 20 VGA to reduce the occurrence of hyperpigmentation or hypopigmentation after cryosurgery or radiowave ablation.
Using a new radiosurgical device (Surgitron; ellman International, Inc), high-frequency low-temperature radiowave ablation allows painless removal of skin lesions, including seborrheic keratosis, common warts, actinic keratosis, solar keratosis, skin tags, and solar lentigos. This unit is unique in that it uses nitrous oxide cartridges rather than an open container of nitrous oxide. For the aesthetic ND, this is a very cost-effective method because the unit charges only when in use.
Other skin lesions that are amenable to treatment with the handheld cryosurgical instrument or with the radiosurgical device are acne vulgaris, acne scars, condyloma acuminata, molluscum contagiosum, and porokeratosis. These techniques work well in treating molluscum contagiosum in children because they are painless and can effectively treat multiple lesions in a short period. Children are amenable to these therapies for the removal of warts because no anesthetic injections are necessary.
It is important as a primary care aesthetic physician that you should differentiate pigmented lesions from possible malignant ones. Skin phototypes I and II are considerably more at risk for melanoma formation. In these patients, it is imperative that you must perform a full-body examination to determine the number of moles. A count of more than 50 moles that exceed 2.0 mm in diameter indicates an increased risk of cancer. However, some patients who are at risk may not have moles (eg, those with red hair or freckles).
Differentiating Benign Pigmented Lesions From Melanomas
It is important to differentiate benign pigmented lesions from melanomas. Always examine the fingers, toes, and plantar and palmar surfaces of the hands, particularly in Sub-Saharan Africans, African Americans, Asians, and Native Americans.
Common moles are less than 5.0 mm in diameter and usually have a distinctively elevated border. Acquired (atypical) moles often exceed 5.0 mm in diameter and appear flat but may actually be elevated when observed using a dermoscope and side lighting.
Melanomas are often dark or variegated in color pattern, with irregular indistinct “fuzzy” borders or a “fried egg” appearance. Six signs of malignant melanoma (the ABCDE mnemonic) include the following: (1) Asymmetrical, in which one half is unlike the other half. (2) Borders are irregular, with scalloped edges. (3) Color is mottled, with shades of brown, black, gray, red, and white. (4) Diameter is wider than the tip of a pencil eraser, usually exceeding 6.0 mm. (5) Elevation, although acral lentiginous lesions may be flat. (6) Enlargement (or evolving over time), which is perhaps one of the most important signs of malignant melanoma, as is a history of bleeding or a tendency to bleed when irritated. If a lesion is suspicious for cancer, the patient should be referred to an oncologist or to a dermatologist who specializes in oncology.
Skin Lesions That are Amenable to Aesthetic Treatment
Sebaceous hyperplasia is a benign skin lesion that usually occurs on the face and forehead, and on close observation they look like small “volcanoes.” When compressed laterally, a droplet of oily fluid is expressed. These lesions chronically drain sebaceous material that irritates the skin, causing reddening, and they have a tendency to spread. They can be treated with the handheld cryosurgical instrument or with the radiosurgical device for ablation of the sebaceous sacs.
Solar lentigos develop over time from exposure to the sun. These brown pigmented areas are often seen in patients who had sun exposure 3 to 4 decades before coming in for evaluation. They are amenable to treatment with the handheld cryosurgical instrument.
Cherry angiomas and cherry hemangiomas are often seen as small red spots on the face, back, chest, arms, and other body surfaces. They are historically benign. Cherry angiomas can be removed with a 1064-nm laser or with the handheld cryosurgical instrument. In the case of cherry hemangiomas, I prefer using the radiosurgical device.
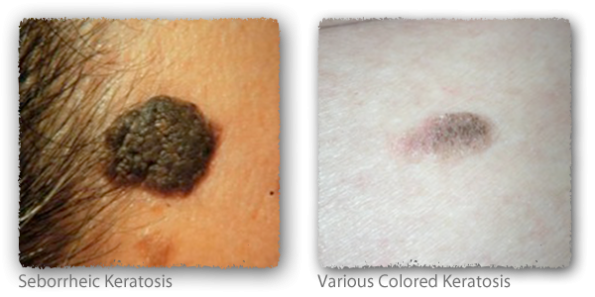
Seborrheic keratosis can appear as various colored, elevated, irregular patches that have a greasy feel. These occur as a result of long-term sun exposure and can be treated with the handheld cryosurgical instrument or with the radiosurgical device.
Skin Lesions That are Amenable to High-Frequency Low-Temperature Radiowave Therapy
The radiosurgical device can be used for aesthetic removal of the following skin lesions: hemangiomas, xanthalasmas, spider veins, dermatofibromas, congenital compound melanocytic nevi, sebaceous hyperplasias, seborrheic keratosis, porokeratosis, and syringomas. The 4.0-MHz frequency applies minimal heat, resulting in less collateral cell damage. Because the high-frequency radiowave passes through the cells, the intracellular water molecules vaporize. The affected cells explode, with little or no damage to the adjacent cells. There is only 10 to 20 µ of heat spread from the point of treatment. The use of this radiowave shortens the procedure time. This modality can also be used to obtain a shave biopsy specimen, and there is no need for stitches. The radiosurgical device allows good visibility and is precise in handling of the tissues. The clinical benefits are reduced postoperative discomfort, minimal scar tissue formation, maximal readability of histological specimens, and enhanced cosmetic results. Other advantages of radiowave therapy are hemorrhage control, a bacteria-free incision, flexible electrode selection, and precise aesthetic management of soft tissues, which avoids scarring.
Xanthalasmas are often seen in patients with hyperlipidemia. However, they can also occur in individuals with normal lipid levels. They usually appear as yellow to orange-yellow plaque beneath the eyes and on the eyelids. These lesions can be removed by careful ablation with the radiosurgical device. As NDs, we should assess patients’ blood lipid levels and prescribe appropriate therapy so that these lesions do not return after removal.
Another frequent benign lesion that we see in our practices from the aesthetic point of view is the compound melanocytic nevi. Some of these lesions may have terminal hair growing in them. Compound melanocytic nevi can be removed using the radiosurgical device and local anesthesia, with minimal to no scarring. Care must be taken to remove only the melanocytic mast cells and go no deeper to avoid scarring and to have a better aesthetic result.
Nevus sebaceous is a benign compound lesion that has a cauliflower-type appearance and often develops on the scalp. These lesions can be removed successfully using the radiosurgical device, without damage to the hair follicle.
In Conclusion
As you can see, there are many indications for the aesthetic removal of benign skin lesions by NDs in their practice. Naturopathic physicians are well trained in coaching patients toward health through proper diet, exercise, and supplementation. We have the ability and training to use aesthetic skin procedures to complement our other treatment regimens to enhance patients’ overall appearance and well-being using the effective aesthetic treatments described herein.
 John Hahn, DPM, ND holds a doctor of podiatric medicine degree. He also received an ND degree from the National College of Naturopathic Medicine in Portland, Oregon. He is certified in foot surgery by the American Board of Podiatric Surgery. Dr Hahn has several published scientific articles and was a contributor to the textbook A Compendium of Podiatric Biomechanics. He has taught as an adjunct instructor at Pioneer Pacific College and Clackamas Community College in Oregon. Dr Hahn was an adjunct professor in the Department of Integrative Medicine at the New York College of Podiatric Medicine, New York City. He is a professional consultant for Heel Inc and is a member of the medical advisory board for GVI. He has delivered lectures to various professional groups for these organizations. Dr Hahn works part-time at the Gresham Cosmetic Laser Center in Troutdale, Oregon, and at Forever Young Medical Spa in Hillsboro, Oregon.
John Hahn, DPM, ND holds a doctor of podiatric medicine degree. He also received an ND degree from the National College of Naturopathic Medicine in Portland, Oregon. He is certified in foot surgery by the American Board of Podiatric Surgery. Dr Hahn has several published scientific articles and was a contributor to the textbook A Compendium of Podiatric Biomechanics. He has taught as an adjunct instructor at Pioneer Pacific College and Clackamas Community College in Oregon. Dr Hahn was an adjunct professor in the Department of Integrative Medicine at the New York College of Podiatric Medicine, New York City. He is a professional consultant for Heel Inc and is a member of the medical advisory board for GVI. He has delivered lectures to various professional groups for these organizations. Dr Hahn works part-time at the Gresham Cosmetic Laser Center in Troutdale, Oregon, and at Forever Young Medical Spa in Hillsboro, Oregon.