Diagnosing Andropause: Vague and Varying Symptoms can Result in Difficult Assessment
Bronner Handwerger, ND
By the time men are between the ages of 40 and 55, they can experience a phenomenon similar to female menopause, called andropause. Unlike women, men do not have a clear-cut indication, such as the cessation of menstruation, to mark this transition. Both, however, are distinguished by a drop in hormone levels. The bodily changes occur very gradually in men and may be accompanied by fatigue, changes in attitudes and moods and/or a loss of energy, sex drive and physical agility.
Andropause is often underdiagnosed because symptoms can be vague and vary among individuals. Some men find it difficult to admit that there’s even a problem, and many times physicians don’t think of low hormone levels as a possible culprit.
These factors often lead doctors to conclude that symptoms were related to other medical conditions (i.e., depression) or were simply related to aging, and often encourage their patients to accept that they are no longer “spring chickens.”
As NDs, we take into account the entire person and work towards restoring balance. As a result, many of our basic therapies work to support and build the endocrine system, since it buffers most of the stress we face over our lifetimes. As the thyroid and adrenal glands begin to weaken, the overall hormonal system is affected. It is very common to see both males and females with lowered hormone levels in the presence of a hypofunctioning thyroid, weak adrenals and poor digestion.
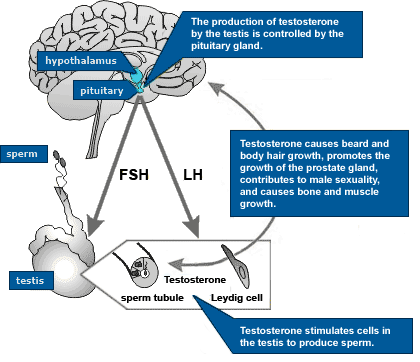 Part of the aging process is the gradual decline in our endocrine system function. Obviously this decline is a natural phenomenon, but when it occurs rapidly, health problems can arise. Uncovering the root cause of this decline is a major part of our task as NDs, so our approach to treating the whole person generally takes into account the multifactorial nature of a weakening endocrine system.
Part of the aging process is the gradual decline in our endocrine system function. Obviously this decline is a natural phenomenon, but when it occurs rapidly, health problems can arise. Uncovering the root cause of this decline is a major part of our task as NDs, so our approach to treating the whole person generally takes into account the multifactorial nature of a weakening endocrine system.
What’s more, studies show that a decline in testosterone can actually put one at risk for other health problems, such as heart disease, metabolic syndrome, low HDL, elevated triglycerides, osteoporosis and even death.
Since all this happens at a time when many men begin to question their values, accomplishments and direction in life, it’s not always obvious that the changes occurring are due to more than psychological factors.
Androgen Deficiency
Beginning at age 30, testosterone begins to drop by approximately 10% per decade. At the same time, there is a rise in sex hormone-binding globulin (SHBG) that binds up free or bioavailable testosterone, rendering it unusable by the body.
Andropause is associated with low levels of bioavailable testosterone. Every man experiences a decline of bioavailable testosterone, but some men’s levels will dip excessively, and when this happens, these men can experience andropausal symptoms.
These symptoms not only impact their quality of life, but may expose them to other, longer-term risks of low testosterone. It is estimated that 30% of men in their 50s will have testosterone levels low enough to cause symptoms or to put them at risk.
As physicians, we must rule out any significant underlying organic causes, especially when working up an individual with androgen deficiency or hypogonadism.
Acquired causes of androgen deficiency can include chemotherapy; damage occurring during surgery or involving the pituitary gland, hypothalamus or testes; head trauma; infections such as meningitis, syphilis or the mumps; radiation therapy to the head or neck; testicular trauma; or tumors of the pituitary gland, hypothalamus or testes.
Other causes to consider are xenoestrogens, poor diet and lifestyle, recreational drugs, history of steroid use, alcohol intake, nutrient deficiencies and heavy metals. The main point is that anything that can affect our adrenals and thyroid is going to have an effect on circulating androgen levels; uncovering any endocrine disruptors that may be present can dramatically improve the ability to return the patient to a healthier state.
Due to many detrimental factors in our environment, a poor daily lifestyle, stress and improper nutrition, I am seeing many younger males – beginning in the late 30s – who show signs of androgen deficiency.
Signs of Deficiency
Among healthy men, there is great variability in testosterone and other hormone levels, so not all will experience the same changes to the same extent. But typical responses to low bioavailable testosterone levels include:
- Low sex drive
- Emotional, psychological and behavioral changes
- Decreased muscle mass
- Loss of muscle strength
- Increased upper and central body fat
- Osteoporosis or decreased bone mass and back pain
- Cardiovascular disease risk
- Low HDL levels
- Elevated triglyceride levels
- Decreased energy
- Difficulty achieving and/or maintaining an erection
- Depression and depression-type symptoms, such as difficulty finding enjoyment in any activity; feeling “grumpy” or “sad”; lacking motivation or desire.
Testing for Andropause
When assessing for andropause, it is important to think about the patient and the symptoms he is reporting. I like to get baseline hormone levels beginning at age 40, but any time a man presents with symptoms at an earlier age, it may be prudent to assess these levels. Doing this serves two purposes: First, it sets a baseline as to where their hormones were, so down the road you can compare with current levels to see any actual rate of decline. Second, it guarantees that you will be able to catch any male who has low androgens years before he may experience symptoms. This allows you to work naturopathically to maintain youthful levels, thereby preventing unwanted effects of low androgen levels.
Saliva, serum and blood testing are performed easily, with many labs offering these services. In my practice, my laboratory workup may include:
- Comprehensive metabolic panel
- Lipid panel
- Cardio CRP
- Homocysteine
- Total and free testosterone, bioavailable
- TSH, free T3 and free T4, TPO (detects autoantibodies directed against the enzyme thyroid peroxidase)
- DHEA sulfate
- Vitamin B12 and folate
- Estradiol
- IGF-1
- Prolactin
- PSA
- Vitamin D
- IGFBP-3
- LH
- Gonadotropin-releasing hormone 1 (GNRH1), also known as Luteinising-hormone releasing hormone (LHRH) (a peptide hormone responsible for the release of FSH and LH from the anterior pituitary. GNRH1 is synthesized and released by the hypothalamus.)
- Urinary toxic elements pre and post provoked.
My approach to androgen deficiency is to first evaluate the patient for underlying causes to determine if this is just a functional deficiency rather than an organic one. Once organic causes have been ruled out, we must begin to flush out the cause, which could be heavy metals, environmental toxicities, adrenal fatigue, thyroid dysfunction, lifestyle, nutrient deficiencies, etc.
What I commonly see occurring is a combination of stress, poor lifestyle and diet, lack of exercise and nutrient deficiency that contribute to lower levels of hormones in general. Also prevalent is the presence of abdominal fat and adipose tissue that allow for greater aromatization, resulting in higher serum estrogen levels.
Elevated levels of estradiol in a male will tend to suppress endogenous testosterone. Care needs to be taken when supplementing DHEA in men, as DHEA can readily convert to estradiol. Some men have more conversion then others due to increased aromatase activity, so it’s important to monitor their levels of estradiol along with the other male hormones.
With patients who are serious or professional athletes, I have noticed the detrimental effects of overtraining. It is not uncommon to see lowered IGF-1, DHEA and testosterone levels with abnormal cortisol patterns in individuals who are very fit and who train hard.
Therapeutic Options for Increasing Androgens
Many therapeutic options are available to us in the treatment of andropause (see the accompanying “short list”). With the ability to uncover so many of the underlying causes, we then have our core therapies that can readily aid in the restoration of balance. Plus, utilizing functional measurements of nutrient status and assessing the body’s burden of environmental toxins help create a base from which we can institute therapeutic protocols.
Questions to Ask Patients
- Do you have a decrease in libido or sex drive?
- Do you have a lack of energy?
- Do you have a decrease in strength or endurance?
- Have you lost weight?
- Have you noticed a decreased enjoyment of life?
- Are you sad or grumpy?
- Are your erections less strong?
- Have you noticed a recent deterioration in your ability to play sports?
- Are you falling asleep after dinner?
- Has there been recent deterioration in your work performance?
If they answer “yes” to question #1 or #7, or answered “yes” to three others, they may have a low testosterone level.
Therapeutic Options for Increasing Androgens (Short List)
- Ginseng
- Tribulus
- DHEA
- Zinc picolinate
- Arginine
- Urtica dioica agglutinin (UDA), which comes from Urtica dioica root (stinging nettle root)
- Maca
- I3C (indole-3-carbinol)
- Glutamine
- Ascorbic acid
- Testosterone transdermal with chrysin (reduces aromatase in the underlying adipose).
 Bronner Handwerger, ND is the medical director of Wellness Kliniek, an integrative health center in San Diego. He served as medical director for the D’Adamo Clinic and as an assistant clinical professor at the University of Bridgeport Naturopathic Medical Center. In addition, Dr. Handwerger served as a panel member for the White House Commission on Complementary and Alternative Medicine. He enjoys working with a wide range of patients, and specializes in the naturopathic approach to endocrinology, oncology and internal medicine.
Bronner Handwerger, ND is the medical director of Wellness Kliniek, an integrative health center in San Diego. He served as medical director for the D’Adamo Clinic and as an assistant clinical professor at the University of Bridgeport Naturopathic Medical Center. In addition, Dr. Handwerger served as a panel member for the White House Commission on Complementary and Alternative Medicine. He enjoys working with a wide range of patients, and specializes in the naturopathic approach to endocrinology, oncology and internal medicine.
References
Bhasin S: Effects of testosterone administration on fat distribution, insulin sensitivity, and atherosclerosis progression, Clin Infect Dis 37:S142–S149, 2003.
Chahal HS and Drake WM: The endocrine system and ageing, J Pathol Jan;211(2):173-80, 2007.
Conley KE et al: Mitochondrial dysfunction: impact on exercise performance and cellular aging, Exerc Sport Sci Rev 35(2):43-49, 2007.
Genazzani AR et al: Long-term low-dose dehydroepiandrosterone replacement therapy in aging males with partial androgen deficiency, Aging Male Jun;7(2):133-43, 2004.
Hormone Research Center and School of Biological Sciences and Technology, Chonnam National University, Republic of Korea.
Köhn FM: Testosterone and body functions, Aging Male Dec;9(4):183-8, 2006.
Kratzik CW et al: Hormone profiles, body mass index and aging male symptoms: results of the Androx Vienna Municipality study, Aging Male Sep;7(3):188-96, 2004.
Kratzik CW et al: The impact of age, body mass index and testosterone on erectile dysfunction, J Urol Jul;174(1):240-3, 2005.
Meinhardt UJ and Ho KK: Modulation of growth hormone action by sex steroids, Clin Endocrinol Oct;65(4):413-22, 2006.
Miner MM and Seftel AD: Testosterone and ageing: what have we learned since the Institute of Medicine report and what lies ahead?, Int J Clin Pract Apr;61(4):622-32, 2007.
Moncada I: Testosterone and men’s quality of life, Aging Male Dec;9(4):189-93, 2006.
Phillips GB et al: The association of hypotestosteronemia with coronary artery disease in men, Arterioscler Thromb May;14(5)701-6, 1994.
Tenover JS: Effects of testosterone supplementation in the aging male, J Clin Endocrinol Metab Oct;75:1092-98, 1992.
Vermeulen A: Diagnosis of partial androgen deficiency in the aging male, Ann Endocrinol (Paris) Apr;64(2):109-14, 2003.
Webb CM et al: Effects of testosterone on coronary vasomotor regulation in men with coronary heart disease, Circulation 100:1690-1696, 1999.
Zmuda JM et al: Longitudinal relation between endogenous testosterone and cardiovascular disease risk factors in middle-aged men. A 13-year follow-up of former Multiple Risk Factor Intervention Trial participants, Am J Epidemiol 146(8): 609-617, 1997.