Menopause Support On All Levels: Can Hot Flashes Be a Spiritual Experience?
Robin DiPasquale, ND, RH (AHG)
Memoirs of a Perimenopausal Woman
I’m lying in my bed at night, sound asleep, deep in a dream. From somewhere comes a feeling in my dantian—a clicking sensation, like a switch being turned. In my subtle awakened state, I recognize this familiar feeling and begin to breathe, allowing my mind to quiet, and bring myself deeper into my being, waiting for insights. From there, warmth begins to spread out in concentric circles throughout my entire torso, through my neck to my head, and down my arms and legs to the extremities. A few minutes later, all over my body, my skin is covered with moisture. From the core where it all began, the sensation of warmth recedes, and the rest of the body follows. My mind is present, yet merged with the deep quiet in the darkness of the night. Moments later, sleep has come again, and I’m dreaming. At times, the clicking sensation occurs in my heart center, with the warmth spreading outward from there. During the day, it is a little more difficult to pause and go deep, so I call upon the nighttime practice to guide me within, while maintaining a connectedness to whomever I am with and whatever I am tending to. Yet, still, it is a reminder to go deeper, to listen, and to engage in life from that place of connection with spirit.
The Menopausal Transition
Menopause has been occurring for women always, even before it was given the name. This is a time of transition, from the archetypal mother to the archetypal crone, the wise woman.
This time in a woman’s life is when the levels of hormones that have been in place for reproduction begin to diminish, triggering a cascade of physiological events. In Western medicine, it is understood that the ovarian estrogen production, primarily estradiol, diminishes markedly through menopause. Estrogen is then stored in adipose tissue, derived from the conversion of androstenedione to estrone. Therefore, the more adipose tissue present, the more conversion occurs, and the more estrone is produced and available to the body.
Hot flashes are the most common menopausal symptom, with up to 85% of women experiencing them; 45% of women experience them for up to 10 years.1 That’s a lot of hot flashing. This vasomotor response, from the thermoregulatory centers in the hypothalamus, is thought to result from lowered estrogen levels, which then trigger increased FSH production from the anterior pituitary gland in an attempt to signal the follicles in the ovaries to respond. We have to wonder why it could take up to ten years for the system to find its equilibrium, for the hypothalamus and pituitary glands to understand that the ovaries are just not able to respond any longer. Another theory is that hot flashes stem from an imbalance in beta-endorphins and other opiates in the brain, possibly triggered by decreased estrogen and/or progesterone levels, influencing the temperature regulation center.2 Cultural attitude may play a part in the prevalence of hot flashes and other menopausal symptoms, as we see women outside of Western cultures reporting fewer or no episodes.
Stress as a Factor
This transition into menopause could/should
be relatively easy and symptom-free; however, the overall imbalances brought on by the stressors of daily life in this current time can explain some of what is behind the challenging collection of physical, mental, and emotional symptoms that may arise, including hot flashes. Since the adrenal glands constitute the main source of androstenedione, adrenal function plays a significant role in how well women transition through menopause. The more the adrenal glands are called upon to respond to stress, the less available they are to take up the job of assisting in this menopausal transition. Supporting the adrenal glands leading up to and through menopause can diminish symptoms by bringing about more overall balance.
Herbal Support for Hot Flashes
Using herbal support doesn’t take away from or interfere with the inner transformation that is occurring on many levels. Herbal support can help us to be more present in our daily lives and to get the rest needed each night for rejuvenation and vitality. We can approach herbal support from both the Western herbal perspective and that of the Traditional Chinese Medicine (TCM )perspective; the two have some overlap.
Western Herbal Medicine
In the Western model, the herbs most frequently considered for diminishing hot flashes fall into the categories of phytoestrogens, cooling herbs, nervines, liver herbs, and herbs to stabilize blood vessels and the cardiovascular system.
Actea racemosa (black cohosh) has celebrity status as the menopausal herb, made famous in Germany. When needing to quiet the hot flashes, just a few drops of black cohosh tincture several times a day will often do the job. One note for perimenopausal women is that the use of black cohosh during this time may encourage the body to continue menstruating.
Well known phytoestrogenic herbs include Trifolium pratense (red clover) and Medicago sativa (alfalfa). Consider a tea of Trigonella foenum-graecum (fenugreek) seeds, infused for 5-10 minutes, during the day or just before bed. Glycyrrhiza glabra (licorice) works via phytoestrogenic action and support of the adrenal glands. Be careful with this herb after 2 pm, as it may disrupt sleep.
Panax quinquefolius (American ginseng) is both cooling and nutritive. It supports adrenal glands, and has some effects on the cardiovascular system. Salvia officinalis (sage) can decrease the frequency and intensity of hot flashes, and diminish the amount of sweating. Use judiciously, since sweating is how the body releases excess heat. The essential oil of Salvia sclera (Clary sage) can be put in a spritzer bottle and used as needed. Some women use their spritzer every hour, while others use it every time they flash. One of my favorite combination oils for hot flashing is composed of Clary sage and Vetiveria zizanoides (vetiver), used for grounding and connecting to the earth. An often overlooked herb for hot flashes is Achillea millefolium (yarrow), which will decrease episodes of flashing, as well as bring many other healing actions to the body. Other cooling herbs to consider include Hibiscus sabdoriffa (hibiscus flowers), Althaea officinalis (marshmallow) and, of course, Mentha spp (mint), which can be included fresh in food or as a tea made from fresh or dry leaves. Stellaria media (chickweed) and the state flower of Wisconsin, Viola odorata (sweet violet), eaten in salads or taken as a tea or tincture, are also excellent cooling herbs.
Tilia tomentosa (linden) is one of two nervines at the top of my hot flash management list. Linden can be used as a tea of the flowers, which is also cooling through its mucilaginous properties, or used as a gemmotherapy bud preparation. Leonurus cardiaca (motherwort), however, is the mother of all nervines for this time of life. It also offers the added benefit of cardiovascular support. Motherwort is very bitter, so is often used as a tincture combined with linden. Another bitter nervine worthy of our attention is Verbena officinalis (hastata), which quiets that inner state as the alchemy takes us down this path of transformation. Rina Nissin, a Swiss nurse and herbalist, wrote in her book back in 1984 of her use of the bud extract (gemmotherapy) of Viscum album (mistletoe), an overlooked nervine, as well as Ribes nigrum (black currant), which, by supporting the adrenal glands, can help abate hot flashes. She also discussed another nervine, Melissa officinalis (lemon balm), the cardiovascular support of Crategus oxycantha (hawthorn), and the cooling effects of Nymphae odorata (water lily).3
Liver herbs assist in overall detoxification, but also with hormone conjugation. There are many to consider, and we’ve already discussed a few, such as the bitter Leonurus and Verbena, both of which act in this way.
For cardiovascular support, we always start off with Crataegus oxycantha (hawthorn). For blood vessel support, my favorite is the gemmotherapy, Sorbus domestica (service tree), which strengthens the vessel walls and assists in the movement of blood. Consider all herbs that are red in color, the doctrine of signature for blood, including Rosa canina (rose hips), hibiscus flowers, Lycium barbarum (wolfberry), and Ziziphus jujuba (jujube dates), as well as Rosa (the rose), an herb of the deep heart essence.
TCM Energetic Patterns
In TCM, it is postulated that menopause arises from a deficiency of essence, which can lead to deficient blood and yin, as well as deficient qi. The deficiency of essence can originally arise from a pattern of excess. The use of herbs is determined according to the energetic patterns that are out of balance, replenishing a deficiency or quieting an excess. These patterns, often numbering more than one in a person, are identified in each individual. Through understanding the patterns present, therapeutics can be selected that assist in bringing the person back to balance. Diet, lifestyle, acupuncture and herbal medicine can all be supportive when chosen appropriately. To understand the details further, I borrow from Leslie Tierra, acupuncturist and herbalist, and share some of her explanations.4
According to Tierra, there are two patterns of excess—stagnant qi/accumulation
of phlegm and stagnant blood. Symptoms of stagnant qi/accumulation of phlegm include feelings of fullness in the epigastrium, belching, nausea, no appetite, feeling of oppression in the chest, obesity, moodiness and depression. This can be seen in women who are busy, pushing their adrenal glands, and upon entering perimenopause, begin to have digestive symptoms that weren’t necessarily a problem in earlier years. Symptoms of stagnant blood include menses that may stop for a long time and then start again, along with clots and dark menstrual blood, mental restlessness, insomnia, hot flashes, and possible abdominal or menstrual pain.
For women with hot flashes who are in an excess state and who maintain good energy, no matter the frequency or intensity of the flashing, the goal is to clear heat, tonify the blood, and support the kidney essence.
goal is to clear heat, tonify the blood, and support the kidney essence.
Herbs that clear uprising heat include Coptis, scute, Gardenia, and moutan.
Blood tonic herbs include Dang gui and white peony.
Kidney essence supporting herbs include Rehmannia, Dioscorea, Cornus and Epimedium.
With deficiency, there are five possible patterns—deficient kidney yin, deficient kidney yang, deficient kidney yin and yang, deficient kidney and liver yin with liver yang rising, and kidneys and heart not harmonized. The array of differentiating symptoms are beautifully and clearly described in Leslie’s book.
In hot flashes of the deficient state, there is low energy, fatigue, reduced immunity, weakness, dryness, and other deficiency signs, depending on the patterns. These women require herbs to tonify the yin, clear deficient heat, regulate liver qi, tonify the blood, and mildly tonify kidney yang.
- Yin tonic herbs include Ophiopogon, asparagus root, and American ginseng.
- Herbs that clear deficient heat and support yin include Anemarrhena.
- Herbs that regulate liver qi include Bupleurum and white peony.
- Blood tonic herbs include cooked Rehmannia, Dang gui, and lycii.
- Mild kidney yang tonic herbs include Epimedium and Cuscuta.
Food and Drink
In addition to herbal support, what you drink and eat each day influences your menopausal journey. Drink plenty of water, choosing it cool to warm, as you like. Herbal teas can cool things down, especially using hibiscus flowers with Rosa canina (dog rose), and, for the cooling polysaccharides, Malva spp or marshmallow. Linden also has mucilaginous properties. Take a pause from alcohol, coffee, and chocolate, as they are too stimulating and too heating.
Foods that contain estrogen-like compounds can be supportive. Two top phytoestrogen foods are pomegranate and dates. Phytoestrogens are found in flax seeds, all beans (including soy, which is more bioavailable in fermented or cultured preparations), legumes, and seeds. Healthy gut flora is essential for converting the lignans in these foods to a usable form. Which foods are best to avoid or include in the diet will vary for each individual woman, depending on her energetic patterning. In general, avoiding hot, spicy foods, refined flour, junk foods, processed foods, and sugar can assist in bringing about better balance. Stimulants like coffee and chocolate can aggravate, as can alcohol. If a congested liver pattern is present, eliminate nuts (walnuts are okay), avocados, dairy products, chips, fried foods, turkey, vinegar, and excessive red meat. With a depleted essence pattern, excessive fruits, fruit juices, and raw foods can aggravate.
Supplemental Support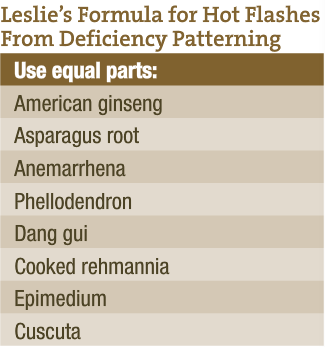
Vitamin E, magnesium, and B vitamins, especially B6, help to minimize the stress response and support cardiovascular integrity, thus are effective allies during the peri- and postmenopausal years. Gamma oryzanol, a ferulic acid extract from grains, particularly rice, dosed at 100 mg TID, has shown effectiveness in diminishing hot flash frequency and intensity.5
Building the Foundation
In addition to herbal support and your daily food and drink, taking care each day to nourish oneself emotionally, energetically, and spiritually becomes essential. When crafting one’s daily schedule, include the essentials for maintaining a solid foundation. Examples include providing a quiet, contemplative or meditative time, a period for exercise, preferably outside, four or more times a week, taking time to pause while eating meals, and scheduling in adequate time for sleep. As you can see, menopause is a time to pause, to take care of oneself, and to make oneself a higher priority on the to-do list. Getting all of these foundational aspects of one’s life in place requires attention; what a woman used to be able to do on automatic pilot can no longer be sustained.
Menopause is appropriately named; it is a time when there is a pause in menstruation. This pause, however, can be taken beyond menstruation, beyond the female reproductive system, and applied to all aspects of life. It may be a time to pause in one’s work life, to slow things down socially, to schedule less, or to decrease the demands placed on oneself by others, or the demands one places on herself. A time to pause can signify a time to re-evaluate all that one does, and reprioritize. It is a time of great inner change, an alchemical transformation, and women may want to partially withdraw from their outer life to spend time exploring and restoring their inner self. And, in this way, hot flashes can be a spiritual experience.

Dr Robin DiPasquale ND RH(AHG)
Robin DiPasquale, ND, RH (AHG) earned her degree in naturopathic medicine from Bastyr University in 1995 where, following graduation she became a member of the didactic and clinical faculty. For the past eight years she has served at Bastyr as department chair of botanical medicine, teaching and administering to both the naturopathic program and the bachelor of science in herbal sciences program. Dr DiPasquale is a clinical associate professor in the department of biobehavioral nursing and health systems at the University of Washington in the CAM certificate program. She loves plants, is published nationally and internationally, and teaches throughout the U.S. and in Italy on plant medicine. She is an anusara-influenced yoga instructor, teaching the flow of yoga from the heart. She currently has a general naturopathic medical practice in Madison, Wis., and is working with the University of Wisconsin Integrative Medicine Clinic as an ND consultant. [email protected]
References
- Maciocia G. Obstetrics & Gynecology in Chinese Medicine. London, England: Churchill Livingstone; 1998.
- Shoupe D, Lobo R. Endogenous opioids in the menopause. In: Speroff L, Lobo R, eds. Role of Opioid Peptides in Reproductive Endocrinology. New York, NY: Thieme Medical Publishers, Inc; 1987:5(2):199-206.
- Nissim R. Natural Healing in Gynaecology, A manual for Women. New York, NY: Pandora Press in association with Methuen, Inc; 1986.
- Tierra L. Healing With The Herbs Of Life. Berkeley, CA: Crossing Press, a division of Ten Speed Press; 2003.
- Ishihara M. Effect of gamma-oryzanol on serum lipid peroxide levels and climacteric disturbances. Asia Oceania J Obstet Gynecol. 1984;10:317.










