Addressing Mitochondrial Alterations in C9orf72-ALS
SAMANTHA PRYOR, ND
Last year my first submission to NDNR was about microbiome alterations found in amyotrophic lateral sclerosis (ALS). I consider that article is essential reading for any clinician who treats someone suffering with ALS, since neuroinflammation can begin in the gut.1 This neuroinflammation can trigger pathology within the mitochondria, hence the topic of this current article: mitochondrial alterations.
My research into ALS started when my father was diagnosed with this terrible neurodegenerative disease. Unfortunately, I lost my father to this disease, at the young age of 51, between my first and second year of naturopathic medical school. Every year I spent in school and since I graduated in 2019 from the University of Bridgeport College of Naturopathic Medicine, I have dedicated myself to the study of ALS.
Amyotrophic lateral sclerosis, or ALS, is a neurodegenerative condition also known as Lou Gehrig’s disease, in reference to the famous baseball player who eventually succumbed to it. In other countries, ALS is known as motor neuron disease (MND). ALS is a neuromuscular disease that begins in the central nervous system with inflammation that damages the upper motor neurons. Eventually, the inflammation damages the lower motor neurons, leading to muscular weakness and eventual paralysis of the voluntary muscles in the body. The average life expectancy after diagnosis is 2 to 5 years. Without adequate intervention, the ultimate cause of death in all patients with ALS is respiratory failure.
Genetic Testing and Early Treatment
Currently, there are up to 30 known causative genetic links to ALS.2 This is important because each mutation has different sequelae that lead to ALS. As a doctor, I recommend all my patients who have a parent affected by ALS to have genetic testing done. Since my father died from ALS, I practiced what I preach, and in September 2021, I submitted a salivary sample for genetic testing. My result came back heterozygous for the C9orf72 hexanucleotide repeat expansion greater than 30, a result considered pathogenic. The C9orf72 gene mutation is the most common cause of familial ALS, resulting in 40% of known cases; this same mutation also contributes to 25% of all cases of familial frontotemporal dementia (FTD).3 Approximately 10% of ALS is familial; however, these mutations have been found in 15% of sporadic (non-familial) ALS as well.2 Since mutation of the C9orf72 gene is the most common familial cause of ALS, this article will focus on ways this gene mutation impacts mitochondria.
The mitochondria are cellular organelles that are important for ATP production, calcium regulation, lipid metabolism, and apoptosis. A study by Mehta et al found that patients with ALS have dense clusters of mitochondria in the anterior horn where the a-motor neurons are, with presynaptic swelling of the mitochondria in the neurons.4 Furthermore, in ALS patients, the mitochondria are more highly concentrated in the soma (the body of the nucleus) and proximal axon. Expression of the protein Miro1, located on the outer mitochondrial membrane and vital for mitochondrial transport along the axon, is reduced in the spinal cords of ALS patients as well.4 Due to this early manifestation of mitochondrial dysfunction in ALS, this study performed a systematic review and meta-analysis to assess the efficacy of treating the mitochondria in ALS. Mehta et al found that targeting mitochondrial dysfunction with treatment resulted in a statistically significant improvement in survival in ALS, especially when such treatment begins pre-symptomatically.4 Hence, genetic testing is highly important for familial ALS diagnosis; with this knowledge, clinicians can begin early treatments for mitochondrial dysfunction if found with a disease-causing mutation. When the study took out the pre-symptomatic treatments and ran the calculation with treatments for mitochondrial dysfunction at symptom onset and end-stage disease there was no statistically significant improvement in survival.4 However, the authors admit that few studies addressed mitochondrial dysfunction treatments after symptom onset and end-stage disease, and that this is an area that needs more research.4
Further, Mehta et al found that most interventions included in the meta-analysis involved oral administration, while studies using other routes of administration were more efficacious because many patients with ALS have swallowing difficulties.4 In my clinical experience, patients with ALS prefer pills over powder applications, since liquids can become hard for them to swallow without choking. Since I have only practiced in the state of Connecticut, I cannot administer supplements through intravenous applications or by injection and am limited to oral and topical applications.
Effects of C9orf72-ALS on Mitochondria and Fibroblasts
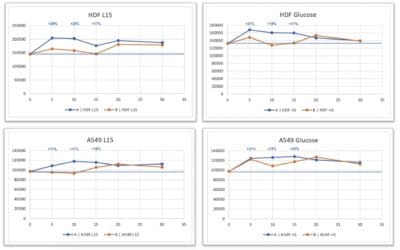
Neurons have high metabolic demands and must remain intact through a person’s lifespan. Therefore, they are susceptible to damage from mitochondrial dysfunction.3 A study by Onesto et al was performed on human C9orf72-ALS fibroblasts that were grown on a galactose medium to switch them to mitochondrial oxidative metabolism for ATP production. This was done since fibroblasts mainly rely on glycolytic metabolism. The study showed that the protein mitofusin 1 was increased 178% compared with controls, which suggests that an altered balance of fission and fusion processes may account for mitochondrial morphology changes observed in C9orf72-ALS fibroblasts.5 The study also measured two2 quantitative morphological parameters for mitochondria length and another for both length and degree of mitochondrial branching. The C9orf72-ALS fibroblasts were significantly lower in both parameters compared to the control. This suggests that the mitochondrial network is altered in C9orf72-ALS fibroblasts.5 The study used electron microscopy for analysis, which revealed some mitochondrial alterations in the lamellar distribution and a deficiency of cristae in C9orf72-ALS fibroblasts.5
To measure the functionality of the mitochondria, Onesto et al ran more tests. First, they measured the mitochondrial membrane potential (MMP) in C9orf72-ALS fibroblasts and found the median MMP value increased 129% over the control value, representing hyperpolarized mitochondria.5 Also, oxygen consumption and ATP levels were significantly increased in C9orf72-ALS fibroblasts over controls.5 The study also found a significant increase in total cellular levels of reactive oxygen species (ROS) and mitochondrial ROS levels in C9orf72-ALS cells over the healthy controls.5
With the increase in ROS levels and the altered morphology found in the C9orf72-ALS fibroblasts, Onesto et al wanted to measure the removal of damaged mitochondria and biogenesis of new ones. The study quantified p62, a marker of autophagic vesical formation, and found a 74% decrease in p62 levels compared to control.5 Fewer autophagic/mitophagic vacuoles were found in Corf72-ALS fibroblasts on electron microscopy, suggesting that autophagy may be activated earlier and at lower levels than usual.5 To test for mitochondrial biogenesis, the study measured mitochondria-encoded NADH dehydrogenase 5 (5MT-ND5), which is a marker for biogenesis; it was found to be significantly higher in C9orf72-ALS fibroblasts compared with controls.5 A regulator of mitochondrial biogenesis, PGC1-a protein, was significantly increased in C9orf72-ALS fibroblasts over controls. Furthermore, mitochondrial mass was increased 172% in C9orf72 fibroblasts compared to control cells.5
Dipeptide Repeat Proteins
For the next finding that affects the mitochondria, a little background information is needed. A competing factor thought to contribute to C9orf72 pathology are dipeptide repeat proteins (DPRs) which are transcribed from the expanded GGGGCC hexanucleotide repeats.6 These repetitive RNA strands can be transcribed into any of 5 DPRs: poly-GA, poly-GP, poly-GR, poly-PA, and poly-PR.6 Several studies have examined DPRs in patients with C9orf72-ALS and have found mostly neuronal cytoplasmic inclusions that contain DPRs. The most common DPRs found, in order, include sense-derived poly-GA, followed by poly-GP and then poly-GR.6 This finding is troubling; according to Smith et al, poly-GR DPRs have been shown to induce mitochondrial damage associated with ALS.3 Also, the poly-GR DPRs preferentially bind to mitochondrial ribosomal proteins.3 Furthermore, several mitochondrial proteins have been shown to interact with C9orf72 proteins in a BioIP proteomics screen, including voltage-dependent anion channel 3 (VDAC3) and translocase of inner mitochondrial membrane 50 (TIMM50), which are members of the inner mitochondrial membrane (IMM) solute carrier family.3 All of this together suggests that DPRs cause significant harm to the mitochondria.
Treating the Mitochondria
Although many drug-based and gene-therapy approaches targeting mitochondrial dysfunction in ALS have shown initial success with animal studies, they have unfortunately been unsuccessful in human clinical trials. Such approaches include the use of coenzyme Q10, dexpramipexole, olesoxime, and creatine.3 As the meta-analysis demonstrated, treatments for mitochondrial dysfunction had statistically significant improvement in survival time when given pre-symptomatically. However, when treatments were initiated either at symptom onset or during end-stage disease, benefits were no longer statistically significant.4 Once again, this elucidates why genetic testing needs to be conducted on family members who have a parent or grandparent either with a current diagnosis of ALS or who have died from ALS. With a confirmatory genetic test, a clinician can begin treatments for mitochondrial dysfunction before symptoms arise.
However, for the many clinicians who do have a symptomatic patient, there are still possible therapies to consider. I would recommend a trial of mitochondrial support like pyrroloquinoline quinone. If no response is obtained, let the patient decide if they want to save money and pursue other treatments like hyperbaric oxygen therapy.
A study by Chen et al analyzed patients with Alzheimer’s disease (AD) and amnestic mild cognitive impairment (aMCI) who were given 40 minutes of hyperbaric oxygen daily for 20 days.7 This 20-day course of hyperbaric oxygen significantly improved cognitive function as assessed by Mini-Mental State Examination (MMSE) and Montreal Cognitive Assessment (MoCA) in AD patients after 1 month.7 In aMCI it improved the MoCA score both 1 and 3 months after treatment, while MMSE scores improved 3 months after treatment.7 Scores on the Activities of Daily Living Scale were also significantly improved in AD patients after 1 and 3 months.7 When compared to control AD patients who received no hyperbaric oxygen treatment, there was a significant improvement in MMSE and MoCA scores after 1 month.7 This treatment might improve C9orf72-ALS because hyperbaric oxygen therapy causes acute oxidative stress on the mitochondria, which stimulates hormesis. The acute oxidative stress will in turn stimulate the mitochondria to upregulate antioxidative defense mechanisms, which over time will improve mitochondria activity and lower ROS levels elevated in the C9orf72-ALS cells when compared to healthy controls.5,8
Finally, since DPRs play such a significant role in the mitochondrial pathology, patients with positive C9orf72-ALS (like me) should regularly water fast to inhibit a protein known as the mechanistic target of rapamycin (mTOR). When insulin is released in response to increased blood sugar, this activates mTOR, which inhibits autophagy in the cell. Water fasting will promote autophagy in hopes of clearing out cytoplasmic inclusions of DPRs. I do this myself for 3 days every 3 months. Keep in mind that any patient who considers water fasting must have good blood sugar control; further, any water fast should be under medical supervision if both doctor and patient agree to add it to their treatment plan.
Thank you for reading my article. Though C9orf72-ALS does play a central, causative role in mitochondrial dysfunction, there are many other known genetic links to ALS. I intend to publish further articles in the future about how these other ALS-causing mutations lead to mitochondrial dysfunction.
[REFS]
- Pryor SJ. Amyotrophic Lateral Sclerosis: Microbiome alterations. NDNR. 2021; 17(7):3.
- Vijayakumar UG, Milla V, Cynthia Stafford MY, et al. A Systematic Review of Suggested Molecular Strata, Biomarkers and Their Tissue Sources in ALS. Front Neurol. 2019;10:400.
- Smith EF, Shaw PJ, De Vos KJ. The role of mitochondria in amyotrophic lateral sclerosis. Neurosci Lett. 2019;710:132933.
- Mehta AR, Walters R, Waldron FM, et al. Targeting mitochondrial dysfunction in amyotrophic lateral sclerosis: a systematic review and meta-analysis. Brain Commun. 2019;1(1):fcz009.
- Onesto E, Colombrita C, Gumina V, et al. Gene-specific mitochondria dysfunctions in human TARDBP and C9ORF72 fibroblasts. Acta Neuropathol Commun. 2016;4(1):47.
- Balendra R, Isaacs AM. C9orf72-mediated ALS and FTD: multiple pathways to disease. Nat Rev Neurol. 2018;14(9):544-558.
- Chen J, Zhang F, Zhao L, et al. Hyperbaric oxygen ameliorates cognitive impairment in patients with Alzheimer’s disease and amnestic mild cognitive impairment. Alzheimers Dement (N Y). 2020;6(1):e12030.
- Schottlender N, Gottfried I, Ashery U. Hyperbaric Oxygen Treatment: Effects on Mitochondrial Function and Oxidative Stress. Biomolecules. 2021;11(12):1827.

Samantha Pryor, ND, graduated from UBCNM in 2019, then completed a 1.5-year residency at her alma mater in March 2021. Serving 6 years in the United States Army as a medic prepared her for the rigors of naturopathic school, where she excelled and graduated at the top of her class. Dr Pryor specializes in generative medicine and nature cure and currently runs her own private practice. She also publishes a weekly video for her YouTube channel: Dr. Sammy Pryor.