Sean X. Hesler, ND
You are in Haiti, the poorest country in the western hemisphere, working in a makeshift clinic with no electricity or running water. The experience is amazing, as each of your patients presents a new challenge to what you learned in school and used in private practice (eg, worms, malaria, and diarrhea). Naturopathic treatments are working well, and you are focusing on the positive by trying to find someone to dig clean wells and build latrines.
Then, Rose comes into your office. Her grandmother tells the heartbreaking story of how she was abandoned and how little she has grown. At 7 months, Rose has now lost head control, and she has fallen off the growth chart. Could it be early cerebral palsy, so common in the region? Or is it gross malnutrition from her diet of flour, cookies, and dirty water because formula is unaffordable? Either way, the answer breaks your heart, and you feel powerless. What can you do?
So You Want to Be a Global Health Physician?
If this story pulls your heartstrings and makes you want to act, I urge you to consider working with a global health organization. With only a few thousand graduates of Council on Naturopathic Medical Education–accredited naturopathic programs and a few hundred students at a time to serve a planet with 7 billion people, we need all the help we can get! The work is endlessly rewarding and always presents new challenges.
Where Do You Start?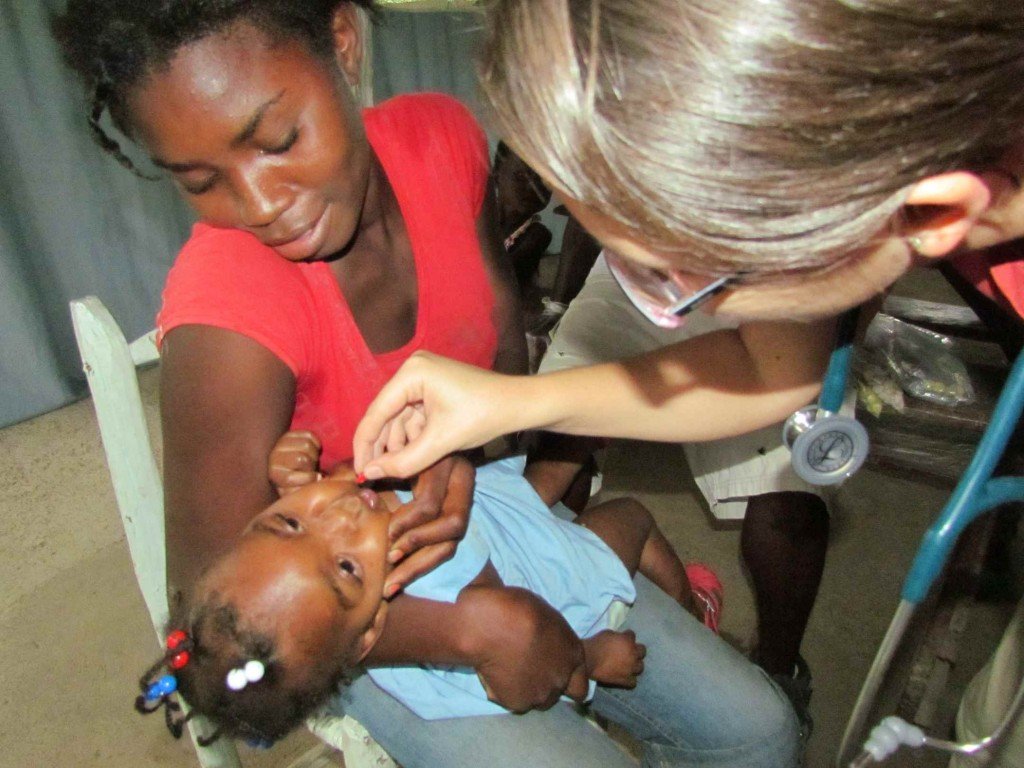
You should ask questions to gauge what you want to do and how you want to do it. Ask yourself the following:
- How involved do I want to be? Should I do local volunteering, a weeklong trip a year, or maybe even a temporary or permanent move?
- Where do I want to work?
- What are my clinical strengths and weaknesses? What might I want to refresh before the trip?
- How do I feel about working around severe acute diseases? Am I comfortable working alongside allopathic physicians?
- Am I prepared to do my best with what I can control and to let go of what I cannot control?
Ask prospective organizations the following questions:
- What is their overall philosophy for delivery of care? Are there any religious requirements for volunteers or recipients of services?
- What are the costs, and do they include meals and transportation?
- Is translation necessary, would it be arranged, and how much would it cost?
- Are there other practitioners working with the organization, locally or on a volunteer basis? Is there a long-term medical presence, or will you do more harm than good by creating a temporary dependence on chronic care?
- Are there any safety concerns, and what security measures are in place?
- What are common and fatal ailments? What are the causes and vectors?
- Which vaccinations are required, and which would I opt for? (Check with the Centers for Disease Control and Prevention.)
- What kind of access is there to medical care, clean water, and food for myself and the local residents?
- What is the scope of practice? Is the organization working with the permission of local health authorities?
- What are some common “cultural beliefs” relating to health and rights?
A Naturopathic Tool Kit to Bring
The following are some high-yield travel-size tools to bring with you in addition to the basics:
- Travel-size homeopathy kit. A few different brands have small kits that contain the most common remedies you will use.
- Vitamin A drops or capsules. The World Health Organization standard capsules are 200 000 IU apiece, but 25 000–IU/drop liquids exist. Vitamin A is great to treat any infection, diarrhea, and skin issues and to prevent and treat night blindness. Standard prophylactic dosing every 6 months is as follows, based on patient age: 50 000 IU for 0 to 6 months, 100 000 IU for 7 to 12 months, and 200 000 IU for older than 1 year.
- Zinc (15-30 mg capsules), to treat any infection, diarrhea, skin issues, connective tissue healing problems, or hyperglycemia.
- A topical anti-infective. Pick your favorite (tea tree, neem, drawing salve, colloidal silver, garlic, honey, etc). You will likely see many skin infections.
- Bug spray, if there are mosquitoes or other biting insects. DEET (diethyltoluamide) is effective, but if you have toxicity concerns, some ND-friendly companies make effective blends. Lemon eucalyptus in particular is an effective mosquito repellant and is widely available.
- Reference guide to cover tropical diseases. The Oxford Handbook of Tropical Medicine (Oxford Medical Publications) and Where There Is No Doctor by David Werner (Hesperian Foundation) are packed with pearls. The Sanford Guide to Antimicrobial Therapy (Antimicrobial Therapy, Inc) is an annually updated guide to prescribing antimicrobial medications and offers side notes.
- Video camera. There are new pocket-size inexpensive digital camcorders to help you capture memories and to take pathology pictures to send to colleagues and specialists for advice!
- An e-reader or tablet with 3G Internet service (check for international use rates). This was a lifesaver in Haiti.
Selected Tropical Diseases
Clinical work in the developing world requires a knowledge of tropical diseases. A comprehensive primer is beyond the scope of this article, but working knowledge of assessment (often without access to laboratory testing) and treatment of intestinal nematodes, malaria, infectious diarrhea, and malnutrition is extremely helpful in your preparation.
The main intestinal nematodes include roundworms (Ascaris), tapeworms (Taenia), whipworms (Trichuris), hookworms (Necator), and pinworms (Enterobious). They have varying vectors, usually fecal-oral, such as eating improperly prepared meats, ingesting soil, or walking barefoot. Roundworms, tapeworms, and whipworms are usually visible in the stool, which makes for an easy clinical diagnosis unless the patient is using a latrine to defecate or is otherwise unable to visualize the stool. Dangerous sequelae include the following:
- Intestinal obstruction by roundworms
- Neurocysticercosis in tapeworms (seizures from fecal-oral ingestion of cysts migrating to the brain)
- Anemia and pica with hookworms (in some areas of the world, it is the leading cause of iron deficiency anemia)
- Rectal prolapse from whipworms (a clinical pearl from Where There Is No Doctor1 is to flip the child upside down and pour cool water onto the rectum)
Albendazole (400-mg single dose) or mebendazole (100 mg twice daily for 3 days) will resolve most intestinal nematode infections. For tapeworms, the following 2 medications (with dosages by age) are superior: niclosamide (500 mg for 0-2 years, 1 g for >2 to 8 years, and 2 g for >8 years) and praziquantel (150 mg for 4-7 years, 300 mg for 8-12 years, and 600 mg for ≥13 years [contraindicated in pregnancy]). Natural treatments I have found effective for nematodes include Juglans nigra, Artemisia annua (only because Vulgaris was not available), and Syzygium aromaticum. In Haiti, I formulated a blend called Werbs (worm herbs) that contained these along with ginger and garlic, with an easily titratable drop dosage based on the patient’s weight. Naturopathic medicine has a rich history of other worm treatments, including bowel purges, milk with raisins soaked in botanicals, and crushed papaya seeds, and the list goes on. Use what you have available! Prevention is focused on building latrines, cleaning up water supplies, properly cooking food, reducing exposure of food to flies, wearing shoes, establishing albendazole prophylaxis programs, and providing access to treatment.
Malaria causes 247 million infections and kills approximately 1 million people annually.2 Owing to the fact that only poor-quality laboratory assessment of malaria existed in our area of Haiti, it was accepted practice to empirically treat fevers of unknown origin as malaria. The diagnostic hallmark is a fever every 2 to 3 days, followed by an intense chill and profuse sweating, depending on the specific type of causative organism. Unfortunately, the deadliest type (falciparum malaria) necessitates prompt treatment (intravenous artesunate is now first-line therapy3), and it has a more frequent fever pattern in most cases. If you have access to laboratory testing, a blood smear will show the parasites inside red blood cells. Allopathic treatment depends on resistance patterns, but most commonly (including in Haiti) chloroquine is used for treatment and prophylaxis. Naturopathically, A annua is a supreme botanical, even when used as a tea4 (thanks to Robert McElroy, ND, for sharing the article). Make sure to send your patient home with a thermometer if he or she does not have one for accurate monitoring of temperature vs subjective feeling related to air temperature.
Diarrhea kills 1.5 million children per year and is the second most common cause of death in children younger than 5 years worldwide.5 Currently, Haiti is experiencing a second wave of its cholera epidemic, which originated from Nepalese United Nations workers in mid 2010 and spread quickly owing to rains and lack of sanitation.6 The exact cause may be difficult to verify, especially without laboratory testing. Do not miss tan “rice-water stools” in endemic areas that may point to cholera, which can be quickly fatal. Vitamin A and zinc are now widely accepted treatments for acute diarrhea, and both have been shown to prevent and reduce the duration of acute diarrhea.7 The use of oral rehydration solution (associated with a 93% reduction in mortality8) obviates intravenous rehydration in all but the most severe cases and is an inexpensive and easily reproduced formula consisting of ½ teaspoon of salt and 6 teaspoons of sugar in 1 L of water. In cases of diarrhea with blood, Giardia (without fever) and Shigella (with fever) are suspect, and appropriate aggressive herbal therapy or antimicrobial medication is indicated. There are many homeopathic remedies to cover various presentations of diarrhea, and far and away the most common and successful I used in Haiti was Podophyllum for painless explosive watery stool with undigested food. Do not be afraid to dose high homeopathic potencies often for acute diarrhea. Locally fermented foods or probiotics can help restore gut flora. To prevent yourself from becoming a patient, I suggest taking probiotics beginning 2 weeks before and throughout the duration of your international travels.
Malnutrition is very easy to spot, and the 2 more worrisome forms, marasmus and kwashiorkor, are especially distinctive. Marasmus is due to a gross lack of calories and protein in the diet, commonly occurring in areas where protein sources are scarce and expensive. It is characterized by a distended abdomen with emaciated limbs and by thinning hair (“skin and bones”). Kwashiorkor is due to protein deficiency, with the major difference being the addition of edema, skin sores, and reddish hair (“skin and bones and water”). With proper treatment, children with kwashiorkor will initially lose weight before regaining it owing to the reduction of edema (this is a positive sign; stay the course). Screening for less obvious malnutrition is best performed with a growth chart, but a middle upper arm circumference (MUAC) of less than 13.5 cm in children older than 1 to 5 years is also diagnostic. A MUAC tape makes measurement easy. Refeeding should be done with calorically dense foods (along with standard vitamins and minerals and, in my opinion, probiotics), while monitoring weight and length weekly. Ready-to-use therapeutic foods, such as Plumpy’Nut (made in France by Nutriset) and Medika Mamba (specific to Haiti), are extremely cost-effective and can be locally produced given the right equipment and quality control. Meds & Foods for Kids (St Louis, Missouri), the company that produces Medika Mamba, is a model of social entrepreneurship and uses grant money to provide Medika Mamba to local aid organizations.
What Happened to Rose?
When Rose was first seen, MamaBaby Haiti (Newberg, Oregon) had just partnered with Meds & Foods for Kids to provide Medika Mamba to patients. After we gave baby Rose a thorough assessment, her grandmother signed a contract saying she would bring the baby back for weekly checkups and would not give Medika Mamba to anyone else. We also decided to give Rose formula because she was younger than 1 year and because breast milk was not available to her. With our fingers crossed, she began gaining weight from the first week and within 3 weeks had regained head control. Now, Rose has a better chance at developing normally, going to school, and breaking the poverty cycle that ultimately caused her circumstance in the first place.
She is the reason why I do what I do. Patients like Rose are why I fight.
 Sean X. Hesler, ND, is the director of professional and academic affairs for Naturopaths Without Borders. He served with MamaBaby Haiti in Cap Haitien as medical director and staff physician for 9 months and accumulated 300 clinical hours with Naturopaths Without Borders while in medical school. Sean has chosen to dedicate his life to medicine for the poor, striving to bridge the gap between NDs/students and underserved communities worldwide.
Sean X. Hesler, ND, is the director of professional and academic affairs for Naturopaths Without Borders. He served with MamaBaby Haiti in Cap Haitien as medical director and staff physician for 9 months and accumulated 300 clinical hours with Naturopaths Without Borders while in medical school. Sean has chosen to dedicate his life to medicine for the poor, striving to bridge the gap between NDs/students and underserved communities worldwide.
References
- Werner D. Where There Is No Doctor. 3rd ed. Berkeley, CA: Hesperian Foundation; 2010.
- World Health Organization. Malaria: fact sheet No. 94. October 2011. http://www.who.int/mediacentre/factsheets/fs094/en/index.html. Accessed October 1, 2011.
- World Health Organization. Guidelines for the Treatment of Malaria. 2nd ed. Geneva, Switzerland: WHO; April 2010.
- Mueller M, Karhagomba I, Hirt H, Wemakor E. The potential of Artemisia annua L. as a locally produced remedy for malaria in the tropics: agricultural, chemical, and clinical aspects. J Ethnopharmacol. 2000;73:487-493.
- World Health Organization. Diarrhoeal disease: fact sheet No. 330. August 2009. http://www.who.int/mediacentre/factsheets/fs330/en/index.html. Accessed October 1, 2011.
- CNN. Vaccarello J. New report links Haiti cholera outbreak to U.N. peacekeepers. May 6, 2011. http://www.cnn.com/2011/WORLD/americas/05/05/haiti.cholera.report/index.html?iref=allsearch. Accessed October 1, 2011.
- Center for Sustainable Development. Zinc & vitamin A: mitigating diarrhea in children. http://www.csd-i.org/zinc-vitamin-a-mitigating-dia/. Accessed October 1, 2011.
- Munos MK, Walker CL, Black RE. The effect of oral rehydration solution and recommended home fluids on diarrhoea mortality. Int J Epidemiol. 2010;39(suppl 1):i75-i87.