Fateh Srajeldin, ND
The purpose of this case report is to present the treatment of severe, long-standing adult onset asthma using alternative therapies, including IV therapy.
The patient had a lengthy history of upper respiratory tract infections that were treated with antibiotics and steroids, and a history of severe asthma between the ages of 36 and 52. The asthma was treated medically with high doses of steroids (local and systemic) and bronchodilators, but was poorly controlled. It severely limited the patient’s lifestyle.
Oral natural treatments, homeopathic remedies and IV treatment containing nutrients, vitamins, minerals, antioxidants and homeopathics over a two-year period has all but eliminated the patient’s need to use inhaled medication and has restored the patient’s capacity to sustain his preferred activities and lifestyle.
Description of the Patient
CP is a 54-year-old man with a warm and gentle disposition. Chief concerns in 2005 included exhaustion; headache; chronic cough with phlegm; chest tightness; shortness of breath; pruritic scalp; arthritis; neck stiffness; back pain; pain in knees, toes and arches; high cholesterol; high blood pressure; and gastrointestinal concerns. He was initially treated with chiropractic treatments for back and joint pain, and on referral from his MD was subsequently treated for asthma.
Presentation and History of Condition
CP’s medical history yielded the following:
- Right mastoiditis at age 8
- Severe colds/flu – MD prescribed antibiotics from age 20
- Right sciatica associated with poor weight-lifting technique from age 27
- Asthma from age 36 – possibly related to flu vaccination
- Right knee operation and chicken pox at age 45
- Recurrence of sciatica at about age 47
- Pneumonia treated with antibiotics at age 48
- Lumpectomy (right thigh) at age 48
- Tonsillitis and sleep apnea at age 52.
The patient’s asthma was diagnosed by his MD and treated with albuterol (1-2 puffs QID/PRN), fluticasone (1-2 puffs BID) and prednisone (5mg tablets, up to 16 tabs per day). The medications failed to control his symptoms, and CP noted that the symptoms’ severity would increase whenever he tried to cut back on the steroids. His medications served to produce temporary relief of symptoms only.
Physical Examination Results
- Lung rales L>R
- Productive cough
- Airways tighten, inflame or fill with mucus
- Coughing, especially at night
- Wheezing
- Shortness of breath
- Cyanotic eyelids and lips
- Inability to finish a sentence
- Chest tightness, pain.
Results for the following lab tests:
- Lung rales L>R
- Productive cough
- Airways tighten, inflame or fill with mucus
Diagnoses
The diagnosis of asthma was based on clinical presentation and patient history. Differentials considered included COPD, congestive heart failure and broncospasm due to chronic sinusitis. Musculoskeletal diagnoses include facet joint irritation of the cervical spine, cervical sprain, neuropathy of the left arm and chronic lumbar strain/sprain.
Treatments
The constituents of the IV treatment have varied somewhat based on changes in the patient’s condition but, in general, have included the following:
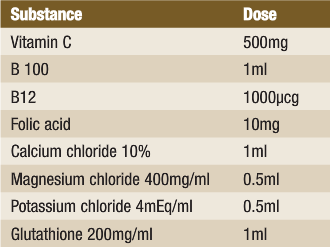 Treatment also included several homotoxicology supplements.
Treatment also included several homotoxicology supplements.
Outcomes
The patient’s musculoskeletal concerns have been responsive to treatment, which is ongoing. CP’s response to IV therapy for his respiratory symptoms has been excellent; in the past year, he has used his albuterol inhaler only two or three times and has completely discontinued the use of fluticasone and prednisone. He is able to conduct his activities of daily living (including regular games of golf) without discomfort.
Discussion
Magnesium has been shown to reduce bronchial hypersensitivity and to be helpful in controlling blood pressure (Schenk et al., 2001; Sanjuliani et al., 1996), and calcium chloride is helpful in reducing blood pressure (Whelton et al., 1997a) as well. Potassium supplementation can also help reduce blood pressure and may be needed to combat hypokalemia secondary to parenteral B12 supplementation (Whelton et al., 1997b; Isaac and Holland, 1992). Vitamin C has been found to be deficient in some asthmatics and has been shown to reduce exercise-induced asthma (Mainous et al., 2000; Cohen et al., 1997). B12 may become deficient with repeated antibiotic use and is used to combat fatigue; B12 also may improve oxygen delivery to the tissues (Werbach, 2000). Folic acid is given conjunctively with B12 because B12 deficiency may be masked by folate. Homeopathic parenteral solutions were given based on clinical presentation to treat the patient’s condition on an energetic level.
Fateh Srajeldin, ND is a graduate of the Ontario College of Naturopathic Medicine. Currently, he is the director of the largest naturopathic clinic of its kind in North America. He has earned certificates and/or membership with various organizations worldwide, including the Canadian Association of Homeopathy; the Board of Directors of Drugless Therapy, Naturopathy; and the Ontario Association of Acupuncture and Traditional Chinese Medicine.
References
Quest Diagnostics. Sedimentation rate chart. Web site: www.questdiagnostics.com/kbase/topic/medtest/hw43353/results.htm
Schenk P et al: Intravenous magnesium sulfate for bronchial hyperreactivity: a randomized, controlled, double-blind study, Clin Pharmacol Ther 69:365-71, 2001.
Sanjuliani AF et al: Effects of magnesium on blood pressure and intracellular ion levels of Brazilian hypertensive patients, Int J Cardiol 56:177-83, 1996.
Whelton PK et al: Efficacy of nonpharmacologic interventions in adults with high-normal blood pressure: results from phase 1 of the trials of hypertension prevention (TOHP). Trials of Hypertension Prev (TOHP) Collab Res Group, Am J Clin Nutr 65:652S-60S, 1997a.
Whelton PK et al: Effects of oral potassium on blood pressure. Meta-analysis of randomized controlled clinical trials, JAMA 277:1624-32, 1997b.
Isaac G, Holland OB: Drug-induced hypokalaemia: A cause for concern, Drugs & Aging 2:35-41, 1992.
Mainous AG et al: Serum vitamin C levels and use of health care resources for wheezing episodes, Arch Fam Med 9:241-5, 2000.
Cohen HA et al: Blocking effect of vitamin C in exercise-induced asthma, Arch Pediatr Adolesc Med 151:367-70, 1997.
Werbach MR: Nutritional strategies for treating chronic fatigue syndrome, Altern Med Rev 5:93-108, 2000.






















