Leslie Solomonian, ND
Holistic sexuality encompasses more than physical sexual and reproductive function (Figure 1). The World Health Organization defines sexual health as “a state of physical, mental and social well-being in relation to sexuality.”1 Human beings are sexual from the moment of birth to the point of death; childhood is a critical time to establish a foundation of sexual self-esteem and expression, the skills to advocate for one’s own pleasure and safety, and a sense of personal sexual responsibility.2
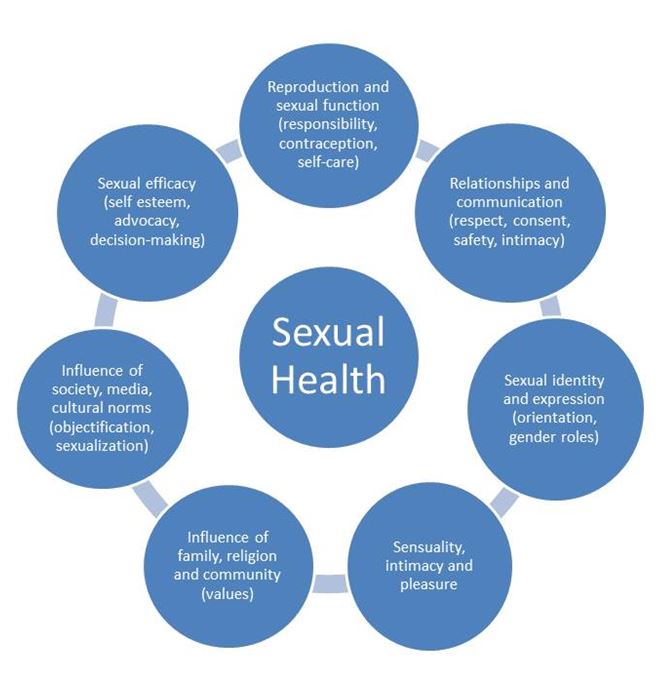
Figure 1. The Many Facets of Sexual Health
The Role of the Parent/Caregiver
Prevention of sexual harms and promotion of positive sexual expression occurs from infancy onward. Although it can be uncomfortable for some, parents are the best primary sexuality educator for their children.2,3 Rather than having one awkward-for-everyone “talk” during puberty, discussing sex early and often reduces discomfort.2 Caregivers can incorporate discussions of sexuality as they arise naturally, addressing a wide range of topics multiple times as the child matures.4 Even open discussions of a non-sexual nature promote healthy sexual expression in youth.5 Nurturing strong attachment from infancy lays the foundation for an open, trusting relationship, which builds self-esteem and protects against sexual harms.
Prompt changing of diapers and teaching good hygiene during toileting teaches children to care for their genitals. Accurate, developmentally-appropriate information should be provided, including correct terminology for all body parts and honestly answering questions about bodily functions. Information can be provided through the lens of the family’s religious, cultural, or philosophical values, and illustrated child-friendly books can help provide information and facilitate discussion (view list of resources in Table 1, online). Developing strategies of decision-making, communication, and consent are transferrable to all facets of life, including sexual well-being.
Masturbation is a safe way for individuals of all ages and genders to learn about their bodies. In adults, masturbation reduces stress and promotes relaxation6; this is likely also true for children. It is normal and natural for infants and children to explore their own bodies, including their genitals.7 Acknowledging and celebrating pleasant sensations establishes positive expectations of pleasure. Children can be taught that touching their genitals feels good and is okay to do in private; culturally-appropriate expectations around privacy should be established without shame.
Perceptions about gender roles are developed early and greatly influence sexual expression. Low perceived sexual power – more commonly experienced by females and youth identifying as lesbian, gay, bisexual, transgender, or questioning/queer (LGBTQ) – is correlated with lack of advocacy for personal pleasure and safety.8,9 Adolescent males who hold traditional views of masculinity are more likely to engage in risky sexual activities, foster less intimacy, and engage in coercion or violence in sexual relationships.10 Modeling has an enormous impact on perceived gender roles; trusted adults of both genders can be encouraged to reflect on their communication styles, expression of affection, and self-advocacy. Conversations can be had with verbal children about their perception of gender roles; the influence of media on gender norms underscores the importance of fostering media literacy from a young age. Caregivers can foster an awareness of and respect for diversity.
Adolescence is a normal and natural time for sexual exploration and experimentation.3 The most recent Youth Risk Behavior Surveillance survey reveals that nearly half of all high school students have had sexual intercourse, while over a third are currently sexually active.11 Adolescents often engage in risky sexual behavior. Factors considered to be “risky” include earlier age at first intercourse, multiple partners, sex without a barrier, sex while under the influence of alcohol or drugs (22.1% had used alcohol or drugs before their last sexual encounter),11 and sex under conditions of coercion or violence. The consequences of these behaviors lead to serious health outcomes associated with sexually transmitted infections (STIs), early pregnancy, and increased likelihood of continuing unhealthy sexual behavior patterns.12,13
Open dialogue with parents promotes healthier sexual expression among youth, both decreasing harm and increasing pleasure.5 When parents talk to youth openly and listen non-judgmentally, youth report feeling closer to their parents and having healthier peer relationships.14 Close, communicative relationships with parents increases the likelihood that sexual activity will occur in a committed relationship, which is correlated with a more pleasurable sexual experience.5 Attributes of self-advocacy, self-esteem, and empathy are associated with orgasm, pleasure, and reciprocity in sexually-active youth, and are fostered by a strong attachment to a trusted caregiver.15 These youth display less risky sexual behavior, including delayed intercourse, reduced frequency of intercourse, decreased risk of sexual abuse and assault, reduced number of sexual partners, and increased use of condoms and other contraceptive methods.16,17
Open and approachable parenting must be balanced with appropriate monitoring and restriction of youths’ leisure activities. As with other risky behaviors, both overly-restrictive parenting and overly-lenient parenting are associated with harmful sexual behaviors. Monitoring by caregivers of youths’ free time is associated with delayed and less risky sexual behavior,5,18 including consumption of sexual content in media. As a powerful source of sexual information and influence (exposure to sexual content is correlated with earlier and riskier sexual activity),19 parental restriction and active co-viewing/listening can protect youth both through limiting exposure and communicating parental values.20,21
Youth typically begin intentionally accessing sexually-explicit media around the time of puberty; this is likely representative of normal curiosity.3 Although concern has been expressed that easy and repeated access to sexually-explicit content may lead to sexual desensitization, this has not yet been supported by the evidence.22 However, pornography dramatically affects perceptions of gender roles, sexual advocacy, pleasure, and consent, and may increase risky or coercive sexual behaviors.9,23,24 Teaching children skills of media literacy from an early age provides the skills to critically evaluate what they may encounter in pornography and other sexually-explicit media. A close relationship with a parent also enables a young person to ask questions about what they see.
Up to 28% of youth have reported engaging in sexting (“sending and sharing sexual photos online, via text messaging, and in person”),25 although it tends to occur at a higher frequency among youth who are already sexual active.3,25 While it may be a lower-physical-risk way of exploring sexual expression, sexting seems to increase the risk of engaging in other higher-risk sexual activities.25 The persistence and shareability of online and digital images can set young people (often females) up for bullying and shaming.27 Some jurisdictions consider images of adolescents shared by adolescents to be child pornography, with devastating consequences for naive perpetrators.28 Caregivers can educate youth about relevant legislation, as well as establish expectations about appropriate decision-making as soon as a young person has the opportunity to engage in social media.26
The Role of the Clinician
While delaying sexual activity reduces risk and promotes positive sexual experiences, youth must be prepared with accurate and comprehensive information in order to make healthy choices. Clinicians can be a source of information, answering children’s questions honestly and age-appropriately.29 A relaxed approach communicates the clinician’s comfort, which normalizes the topic and invites future questions. Myriad written and online resources exist for caregivers, educators, clinicians, and young people. A non-exhaustive list is provided in Table 1, online.
Sexuality-specific anticipatory guidance can be provided at all well-child checks – delivered to the caregiver in the early years, and directly to the youth as the years progress. This requires trust and rapport, best established early in the therapeutic relationship. As with all patients, an open, non-judgmental approach will encourage honesty and thus more opportunity for normalization, education, and motivational interviewing. It is normal for youth to experience curiosity and anxiety around sexual changes; they may have questions about what to expect and how to adjust their self-care. There is a strong association between pubertal changes and self-esteem,30 influenced by media and peers.3 Anticipating questions and providing guidance prior to expected changes occurring can tremendously alleviate any uncertainty or worry a young person may be experiencing. Physical examination of the entire body, including the genitals, facilitates assessment of healthy growth and development, and provides an opportunity to teach the young person about his or her body. Consent can be enabled by establishing this expectation early in the therapeutic relationship, providing education about the relevance, and by including a third party (eg, a parent or an office assistant).
A supportive and normalizing environment is of critical importance, particularly for youth who identify as LGBTQ or who are curious about exploring non-hetero/cis expressions of sexuality.31 There is a higher incidence of depression, suicidality, and substance abuse in LGBTQ youth. LGBTQ youth experience higher rates of violence, coercion and victimization, and demonstrate higher-risk sexual behavior.32 In many cases, home is not a supportive environment; a substantial number of street-involved youth identify as LGBTQ. Clinicians should screen for these concerns, and avoid hetero/cis-normative language and bias.15
Screening for engagement in sexual activity is best done with caregivers absent (caregivers and youth must be appropriately informed of the limits of confidentiality).33 It is important to discuss behaviors as opposed to definitions, since mis-education is common and sexual identity is emerging during adolescence.34 The word “sex” itself may have different meanings to different individuals, meaning penetrative intercourse to some, while overlooking the expression of sexuality through other means. Different activities carry different risks of STI transmission; accurate information must be available in order to reduce risk. Lower-risk behaviors, such as “sexting,” mutual masturbation, and oral sex are common among youth, and may be safer ways of building skills of intimacy, communication, sexual advocacy, and reciprocity.3 Youth can be encouraged to explore words like “virginity,” “abstinence,” and “sex” to frame their personal sexual expression in a way that feels pleasurable, empowering, and safe.9 Table 2 provides some language and strategies for engaging with youth.
Table 2. Strategies for Engaging with Youth Around Sexuality
| Seek information in a respectful manner | |
| “Have you been sexually active with anyone (guys, girls, or both) in the past 6 months?” | |
| “Do you have any concerns or questions about sex?” | |
| “What have you learned about preventing pregnancy and STIs?” | |
| “Do you have any thoughts about birth control?” | |
| Describe how you can help | |
| “I can be a source of information for you, and help provide you with the resources to make healthy decisions.” | |
| Be direct | |
| “HIV can kill you.” | |
| “Getting pregnant when you’re not ready can be devastating to your future.” | |
| “Having sex while you’re drunk or high increases the risk of STIs or pregnancy.” | |
| “Having naked pictures of your girl/boyfriend on your phone could get you in a lot of trouble with the law.” | |
| Address limits of confidentiality | |
| “I will keep anything you tell me confidential unless I’m worried that you or someone else might get hurt. Do you have any questions about what is and isn’t confidential?” | |
| Set goals | |
| “Let’s set up an appointment to talk about options for contraception.” | |
| “Do you think you can have a conversation with your girl/boyfriend about getting tested for STIs?” | |
| “Let’s role-play what you might do the next time you feel pressured to give a blow job.” | |
(Adapted from Adolescent Health Screening and Counseling; Ham P, 2012)43
In one review, more than half of males admitted to wishing they had waited longer to engage in sexual intercourse; most reported feeling pressured, and more than a third reported not wanting to have had sex the first time.35 Just under 10% of high school students have reported physical violence by an intimate partner11; 8% of students have reported being physically forced to have sexual intercourse, with a higher incidence among females.11 Coercion and violence in adolescent relationships have long-lasting impacts on mental and reproductive health, including an increased risk of depression, STIs and unwanted pregnancy, and future patterns of violence.10 Adolescents should be asked about coercion or violence in casual and committed relationships.10 The age of sexual consent varies among jurisdictions; clinicians should also screen for any concerns of this nature.
Forty percent of sexually-active youth reported not having used a condom in their most recent sexual encounter; 12.9% had used no method to prevent pregnancy.11 All youth should be engaged in a discussion around appropriate contraception and prophylaxis, ideally prior to the initiation of sexual activity.36,37 Unintended teen pregnancies predict lower education, unemployment, lower lifetime earnings, single parenthood, depression, and poor infant health,38,39 while STIs contribute to both morbidity and mortality; adolescents account for half of all new STI diagnoses in the United States.40 Long-acting reversible contraceptive methods (such as intrauterine devices) are recommended as the first-line approach to prevent pregnancy,33 although youth need to know that these methods do not protect against STIs. Barrier methods should be used during all adolescent sexual encounters (in addition to any hormonal contraception) to ensure maximal protection against both STIs and pregnancy.37 Marcell et al is an excellent source for strategies to increase condom use in youth.35
Healthcare providers must be aware of STI screening and reporting guidelines in their jurisdiction. American and Canadian guidelines for screening adolescents are largely the same (more detailed guidelines42 can be found on the CDC’s website)41,42:
- All adults and adolescents from ages 13 to 64 should be tested at least once for HIV
- All sexually-active women younger than 25 years should be annually screened for Chlamydia and gonorrhea
- All sexually-active gay, bisexual, and other males who have sex with males (MSM) should be screened at last once a year for syphilis, Chlamydia, and gonorrhea. MSM who have multiple or anonymous partners should be screened more frequently for STIs (ie, at 3 to 6-month intervals).
- Anyone who has unsafe sex or shares injection drug equipment should get tested for HIV at least once a year. Sexually-active gay and bisexual males may benefit from more frequent testing (eg, every 3 to 6 months).
Summary
Young people engage in sexual activity. Optimal sexual health includes responsibility for self, reciprocity toward others, sexual efficacy, and the ability to advocate for both sexual safety and pleasure. In order to promote optimal sexual health, clinicians can encourage open, honest relationships between youth and trusted adults from infancy onward. Clinicians can be a direct source of accurate information and education, and act as a resource for caregivers in providing key messages to young people (Table 3).
Table 3. Key Messages for Children To Foster Healthy Sexuality
| Sexuality is a natural and healthy part of life |
| You have the right to be loved and cared for, and to feel safe and protected |
| Your body is yours; no one else has the right to touch it or comment on it without your consent; sometimes a doctor or a nurse may need to look at or touch your body to make sure you are healthy |
| If you are ever uncomfortable with the way someone is looking at, touching, or talking about your body, tell an adult that you trust |
| Body parts should be called by their correct names |
| It is your responsibility to take care of your body |
| You have the right to have your questions and concerns about your body answered honestly and accurately |
| Masturbation is a natural and healthy way of exploring sexuality, delaying sexual intercourse, and learning about your body |
| You have the right to sexual safety, privacy, and pleasure |
| Others also have the right to sexual safety, privacy, and pleasure; we have the responsibility to express our sexuality in a way that is respectful of others |
| The only true consent is an enthusiastic one |
| You have the right to access confidential healthcare resources regarding sexuality, reproduction, contraception, and health |
| STIs lead to serious consequences and are preventable |
| Abstaining from sexual intercourse is the most effective way to prevent pregnancy and STIs; if you are going to engage in sexual intercourse, a barrier should be used every time |
| Communication and trust are key; if you can’t talk to a potential partner about having sex, you shouldn’t be having sex with that person |
| You are valuable and worthy, no matter whom you love or are attracted to |
Table 1a. Book Resources for Children, Youth and Parents (non-exhaustive list)
| Books for Younger Children |
| Spelman CM. Your Body Belongs to You. Park Ridge, IL: Albert Whitman and Company; 1997. |
| Harris RH. It’s Not the Stork!: A Book About Girls, Boys, Babies, Bodies, Families and Friends. Somerville, MA: Candlewick Press; 2008. |
| Silverberg C. What Makes a Baby. New York, NY: Penguin Random House; 2013. |
| Parr T. The Family Book. New York, NY: Little, Brown and Company; 2010. |
| Harris RH. It’s So Amazing!: A Book about Eggs, Sperm, Birth, Babies, and Families. Somerville, MA: Candlewick Press; 2014. |
| Books for Older Children |
| Dunham K. The Boy’s Body Book: Everything You Need to Know for Growing Up YOU. 3rd ed. Kennebunkport, ME: Cider Mill Press; 2015. |
| Dunham K. The Girls Body Book: Everything You Need to Know for Growing Up YOU. Kennebunkport, ME: Cider Mill Press; 2013. |
| Schaefer V. The Care and Keeping of You: The Body Book for Younger Girls. New revised ed. Middleton, WI: American Girl Publications; 2013. |
| Silverberg C. Sex is a Funny Word: A Book about Bodies, Feelings, and YOU. New York, NY: Penguin Random House; 2015. |
| Harris RH. It’s Perfectly Normal: Changing Bodies, Growing Up, Sex, and Sexual Health. Somerville, MA: Candlewick Press; 2014. |
| Books for Teens |
| Huegel K. GLBTQ: The Survival Guide for Gay, Lesbian, Bisexual, Transgender, and Questioning Teens. Golden Valley, MN: Free Spirit Publishing; 2011. |
| Basso MJ. The Underground Guide to Teenage Sexuality. 2nd ed. Minneapolis, MN: Fairview Press; 2003. |
| Corinna H. S.E.X.: The All-You-Need-To-Know Sexuality Guide to Get You Through Your Teens and Twenties. 2nd ed. Boston, MA: Da Capo Lifelong Books; 2016. |
| Books for Parents |
| Haffner DW. Beyond the Big Talk: A Parent’s Guide to Raising Sexually Healthy Teens – From Middle School to High School and Beyond. Revised ed. New York, NY: Newmarket Press; 2008. |
| Haffner DW. From Diapers to Dating: A Parent’s Guide to Raising Sexually Healthy Children – From Infancy to Middle School. New York, NY: Newmarket Press; 2008. |
| Vernacchio A. For Goodness Sex: Changing the Way We Talk to Teens About Sexuality, Values, and Health. New York, NY: Harper Wave; 2014. |
| Orenstein P. Girls & Sex: Navigating the Complicated New Landscape. New York, NY: HarperCollins Publishing; 2016. |
| Levkoff L, Wider J. Got Teens?: The Doctor Moms’ Guide to Sexuality, Social Media and Other Adolescent Realities. New York, NY: Hachette Book Group; 2014. |
Table 1b. Online Resources for Sexuality Education
| Description | Website |
| Talk About Sex: A resource for youth produced by the Sexuality Information and Education Council of the United States (SIECUS), including a list of online resources | http://www.siecus.org/document/docWindow.cfm?fuseaction=document.viewDocument&documentid=191&documentFormatId=223 |
| Sex, etc: A comprehensive sexuality education website for teens 13- to 19 years old; produced by Rutgers University | http://sexetc.org/ |
| Scarleteen: Sex ed for the real world: An independent, grassroots sexuality and relationships education and support organization and website | http://www.scarleteen.com/ |
| Young Men’s Health: “Carefully researched health information” for teenage boys and young men; produced by the Division of Adolescent and Young Adult Medicine at Boston Children’s Hospital. Includes sections for teens, parents, and practitioners. | http://youngmenshealthsite.org/ |
| Center for Young Women’s Health: “Carefully researched health information” for teenage girls and young women; produced by the Division of Adolescent and Young Adult Medicine at Boston Children’s Hospital. Includes sections for teens, parents, and practitioners. | http://youngwomenshealth.org/
|
| The Trevor Project: “The leading national organization providing crisis intervention and suicide prevention services to lesbian, gay, bisexual, transgender and questioning (LGBTQ) young people ages 13-24” | http://www.thetrevorproject.org/ |
| Amplify: “A project of Advocates for Youth, which champions efforts to help young people make informed and responsible decisions about their reproductive and sexual health” | http://amplifyyourvoice.org/ |
| PFLAG: “The nation’s largest family and ally organization; committed to advancing equality and full societal affirmation of LGBTQ people” | www.pflag.org |
| CDC; Get Tested: Interactive online resource to locate free, fast, and confidential STI testing in the United States | https://gettested.cdc.gov/ |
| Planned Parenthood: “Delivers vital reproductive health care, sex education, and information to millions of women, men, and young people worldwide.” Includes sections for teens, parents, and practitioners. | www.plannedparenthood.org |
| I wanna know!: “A site of the American Sexual Health Association, America’s authority for sexually transmitted infection information.” Includes sections for teens, parents, and educators. | www.Iwannaknow.org |
| SexualityandU: “The ultimate Canadian web site committed to providing accurate, credible and up-to-date information and education on sexual health. An initiative of the Society of Obstetricians and Gynaecologists of Canada.” Includes sections for teens, parents, and practitioners. | http://www.sexualityandu.ca/ |
| Answer: Sex ed, honestly: “Support for parents, practitioners, providing invaluable sexuality education resources to millions of young people and adults every year.” A division of Rutgers University. Includes sections for teens, parents, and practitioners. | http://answer.rutgers.edu/ |
| Family Acceptance Project: “A research, intervention, education and policy initiative that works to prevent health and mental health risks for lesbian, gay, bisexual and transgender (LGBT) children and youth” | http://familyproject.sfsu.edu/ |
| Right From the Start: Guidelines for Sexuality Issues: A resource for promoting healthy sexuality in infants and children; produced by SIECUS | http://www.thetalkinstitute.com/articles/RightFromTheStart_birthto5guidelines.pdf |
 Leslie Solomonian, ND, is an associate professor at the Canadian College of Naturopathic Medicine, where she teaches pediatrics. Leslie also delivers holistic sexuality education programs to adults and youth. She is acutely aware of how deep and broad this topic is; she would have loved to give more attention to many themes, including sexual identity and orientation (including asexuality), the impact of media, the balance between pleasure and safety, and the complex reasons that youth engage in sexual behavior. Any omissions were difficult to make. Leslie encourages readers to view this piece as inspiration for deeper exploration and reading.
Leslie Solomonian, ND, is an associate professor at the Canadian College of Naturopathic Medicine, where she teaches pediatrics. Leslie also delivers holistic sexuality education programs to adults and youth. She is acutely aware of how deep and broad this topic is; she would have loved to give more attention to many themes, including sexual identity and orientation (including asexuality), the impact of media, the balance between pleasure and safety, and the complex reasons that youth engage in sexual behavior. Any omissions were difficult to make. Leslie encourages readers to view this piece as inspiration for deeper exploration and reading.
References
- World Health Organization. Health Topics: Sexual Health. WHO Web site. http://www.who.int/topics/sexual_health/en/. Accessed April 8, 2016.
- Wilson EK, Dalberth BT, Koo HP, Gard JC. Parents’ perspectives on talking to preteenage children about sex. Perspect Sex Reprod Health. 2010;42(1):56-63.
- Fortenberry JD. Puberty and adolescent sexuality. Horm Behav. 2013;64(2):280-287.
- Martino SC, Elliott MN, Corona R, et al. Beyond the “big talk”: the roles of breadth and repetition in parent-adolescent communication about sexual topics. Pediatrics. 2008;121(3):e612-e618.
- Parkes A, Henderson M, Wight D, Nixon C. Is parenting associated with teenagers’ early sexual risk-taking, autonomy and relationship with sexual partners? Perspect Sex Reprod Health. 2011;43(1):30-40.
- Leonard A. An Investigation of Masturbation and Coping Style [poster]. 38th Annual Western Pennsylvania Undergraduate Psychology Conference. Slippery Rock, PA; 2010.
- Finkelstein E, Amichai B, Jaworowski S, Mukamel M. Masturbation in prepubescent children: a case report and review of the literature. Child Care Health Dev. 1996;22(5):323-326.
- Haberland N, Rogow D. Sexuality education: emerging trends in evidence and practice. J Adolesc Health. 2015;56(1):S15-S21.
- National Public Radio; Fresh Air. ‘Girls & Sex’ And The Importance Of Talking To Young Women About Pleasure. Published March 29, 2016. NPR Web site. http://www.npr.org/sections/health-shots/2016/03/29/472211301/girls-sex-and-the-importance-of-talking-to-young-women-about-pleasure. Accessed April 8, 2016.
- De Koker P, Mathews C, Zuch M, et al. A systematic review of interventions for preventing adolescent intimate partner violence. J Adolesc Health. 2014;54(1):3-13.
- Eaton DK, Kann L, Kinchen S, et al. Morbidity and Mortality Weekly Report (MMWR) Youth Risk Behavior Surveillance – United States, 2011. MMWR CDC Surveill 2012;61(SS04);1-162.
- Oudekerk BA, Allen JP, Hafen CA, et al. Maternal and Paternal Psychological Control as Moderators of the Link between Peer Attitudes and Adolescents’ Risky Sexual Behavior. J Early Adolesc. 2014;34(4):413-435.
- Kastbom ÅA, Sydsjö G, Bladh M, et al. Sexual debut before the age of 14 leads to poorer psychosocial health and risky behaviour in later life. Acta Paediatr. 2015;104(1):91-100.
- Akers AY, Holland CL, Bost J. Interventions to improve parental communication about sex: a systematic review. Pediatrics. 2011;127(3):494-510.
- Schalet AT, Santelli JS, Russell ST, et al. Invited commentary: broadening the evidence for adolescent sexual and reproductive health and education in the United States. J Youth Adolesc. 2014;43(10):1595-1610.
- Rupp R, Rosenthal SL. Parental influences on adolescent sexual behaviors. Adolesc Med State Art Rev. 2007;18(3):460-70, vi.
- Sutton MY, Lasswell SM, Lanier Y, Miller KS. Impact of parent-child communication interventions on sex behaviors and cognitive outcomes for black/African-American and Hispanic/Latino youth: a systematic review, 1988-2012. J Adolesc Health. 2014;54(4):369-384.
- Dittus PJ, Michael SL, Becasen JS, et al. Parental Monitoring and Its Associations With Adolescent Sexual Risk Behavior: A Meta-analysis. Pediatrics. 2015;136(6):e1587-e1599.
- Collins RL, Elliott MN, Berry SH, et al. Watching sex on television predicts adolescent initiation of sexual behavior. Pediatrics. 2004;114(3):e280-e289.
- Brown JD, L’Engle KL, Pardun CJ, et al. Sexy media matter: exposure to sexual content in music, movies, television, and magazines predicts black and white adolescents’ sexual behavior. Pediatrics. 2006;117(4):1018-1027.
- Parkes A, Wight D, Hunt K, et al. Are sexual media exposure, parental restrictions on media use and co-viewing TV and DVDs with parents and friends associated with teenagers’ early sexual behaviour? J Adolesc. 2013;36(6):1121-1133.
- Landripet I, Štulhofer A. Is Pornography Use Associated with Sexual Difficulties and Dysfunctions among Younger Heterosexual Men? J Sex Med. 2015;12(5):1136-1139.
- Rothman EF, Adhia A. Adolescent Pornography Use and Dating Violence among a Sample of Primarily Black and Hispanic, Urban-Residing, Underage Youth. Behav Sci (Basel). 2015;6(1):pii: E1.
- Stanley N, Barter C, Wood M, et al. Pornography, Sexual Coercion and Abuse and Sexting in Young People’s Intimate Relationships: A European Study. J Interpers Violence. pii: 0886260516633204. [Epub ahead of print]
- Ybarra ML, Mitchell KJ. “Sexting” and its relation to sexual activity and sexual risk behavior in a national survey of adolescents. J Adolesc Health. 2014;55(6):757-764.
- Rice E, Rhoades H, Winetrobe H, et al. Sexually explicit cell phone messaging associated with sexual risk among adolescents. Pediatrics. 2012;130(4):667-673.
- Korenis P, Billick SB. Forensic implications: adolescent sexting and cyberbullying. Psychiatr Q. 2014;85(1):97-101.
- Lorang MR, McNiel DE, Binder RL. Minors and Sexting: Legal Implications. J Am Acad Psychiatry Law. 2016;44(1):73-81.
- Canadian Paediatric Society Adolescent Health Committee. Harm reduction: An approach to reducing risky health behaviours in adolescents. Paediatr Child Health. 2008;13(1):53-56.
- Labbrozzia D, Robazzaa C, Bertollo M, et al. Pubertal development, physical self-perception, and motivation toward physical activity in girls. J Adolesc. 2013;36(4):759-765.
- Society for Adolescent Health and Medicine. Recommendations for promoting the health and well-being of lesbian, gay, bisexual, and transgender adolescents: A position paper of the Society for Adolescent Health and Medicine. J Adolesc Health. 2013;52(4):506-510.
- Coker TR, Austin SB, Schuster MA. Health and health care of lesbian, gay, and bisexual adolescents. Annu Rev Public Health. 2010;31:457-477.
- The Society for Adolescent Health and Medicine, Burke PJ, Coles MS, et al. Sexual and reproductive health care: a position paper of the Society for Adolescent Health and Medicine. J Adolesc Health. 2014;54(4):491-496.
- Steensma TD, Kreukels BP, de Vries AL, Cohen-Kettenis PT. Gender identity development in adolescence. Horm Behav. 2013;64(2):288-297.
- Marcell AV, Wibbelsman C, Seigel WM; Committee on Adolescence. Male adolescent sexual and reproductive health care. Pediatrics. 2011;128(6):e1658-e1676.
- Upadhya KK. Contraception for adolescents. Pediatrics. 2013;34(9):384-394.
- Nierengarten M. Contraception guidelines for adolescents. Contemp Pediatr. 2015;32(6):18-22.
- Unplanned Pregnancy Among Unmarried Young Women. The National Campaign to Prevent Teen and Unplanned Pregnancy. October 2012. Available at: https://thenationalcampaign.org/sites/default/files/resource-primary-download/briefly-unplanned-pregnancy-among-unmarried.pdf. Accessed April 10, 2016.
- Child Trends Databank. Unintended Births. Last updated September 2013. Available at: http://www.childtrends.org/?indicators=unintended-births. Accessed April 10, 2016.
- Centers for Disease Control and Prevention. Sexual Risk Behaviors: HIV, STD, & Teen Pregnancy Prevention. Last updated April 15, 2016.CDC Web site. http://www.cdc.gov/healthyyouth/sexualbehaviors/. Accessed April 10, 2016.
- Allen UD, MacDonald NE; Canadian Paediatric Society, Infectious Diseases and Immunization Committee, Infectious Diseases and Immunization Committee. Sexually transmitted infections in adolescents: Maximizing opportunities for optimal care. Paediatr Child Health. 2014;19(8):429-433.
- Centers for Disease Control and Prevention. STD and HIV Screening Recommendations. Last updated February 11, 2016. CDC Web site. http://www.cdc.gov/std/prevention/screeningreccs.htm. Accessed April 10, 2016.
- Ham P, Allen C. Adolescent Hhalth screening and counseling. Am Fam Physician. 2012;86(12):1109-1116.