Diane Angela Fong, ND
“Miasm” is the term Hahnemann used to describe an inherited predisposition for certain physical and/or mental dysfunctions.1 Just as biological genes are carried down from parent to child, miasms can be inherited in a similar fashion. In infants or young children with atopic dermatitis, also known as eczema, I often find that the Psora miasm has been inherited. Even after improving diet and lifestyle, and providing gastrointestinal support, detoxification, botanical medicine, and nutrient supplementation, many of these patients will only find about 50-85% relief, or their improvement is not long-lasting. These modalities are important, however, because they can clear the “obstacles to cure,”2 making way for a well-prescribed homeopathic remedy to address the miasm.
The Psora Miasm
Hahnemann described the Psora miasm as the “intolerable itch.”1 He believed that the miasm originated from the suppression of leprosy, that occurred from 600 BC to the Middle Ages, and that it has been carried down into the present day.1 Psora expresses itself with external skin conditions that originate from a malfunction in the primary routes of elimination. Psoric patients will find that whenever they are unhealthy, they will always manifest external skin symptoms. The chief Psoric remedies include Sulphur, Natrum muriaticum, Lycopodium, Graphites, and Psorinum, among many others. These remedies must always be considered when treating a child with eczema.
The following 2 cases are great examples of how a well-chosen Psoric remedy fueled the healing process. In the first case, I first prescribed Pulsatilla. This remedy led to some improvement, but I later found that the Psoric remedy, Psorinum, stimulated the most healing. In the second case, I started with Sulphur 6C, and found that increasing the potency to 30C helped move the case forward.
Case Study 1
David, a 13-month-old male, presented to my clinic in September 2015 with severe atopic dermatitis, nasal congestion, poor sleep, and diminished appetite.
First Visit
History
The patient’s mother reported that David had eczema since birth. He had mild jaundice at birth. The patient consumed breast milk and cow’s milk formula, and his diet consisted of oatmeal with mashed bananas, rice pasta with tomato or cheese sauce, rice and vegetables, cheerios, grapes, and tomatoes. The patient’s sleep was restless, but he was able to sleep through the night when he took hydroxyzine. David’s older sister has multiple food allergies, asthma, and eczema. His father, maternal aunt, and uncle have eczema, and his mother had mild asthma in college.
Homeopathic
The patient does not like being in a hot, stuffy room. He loves music and being outdoors. He does not like being left alone, and he is very sensitive to loud sounds and jarring noises. He loves bread, salty food, cheese, chocolate, eggs, meat, and milk. He likes to sleep without covers on, and he prefers sleeping on his right side or on his abdomen with his legs tucked up. He needs to sleep with 2 stuffed animals. David’s mother had to carry him to soothe him during the visit.
Objective
His skin was erythematous, edematous, dry, oozing with a thick, yellow exudate, and he had some visible open wounds from scratching. The patient’s entire body was covered in eczema (Figure 1). He was visibly uncomfortable at the visit. His left ear canal was completely impacted with cerumen. Mild ronchi were heard upon inspiration bilaterally.
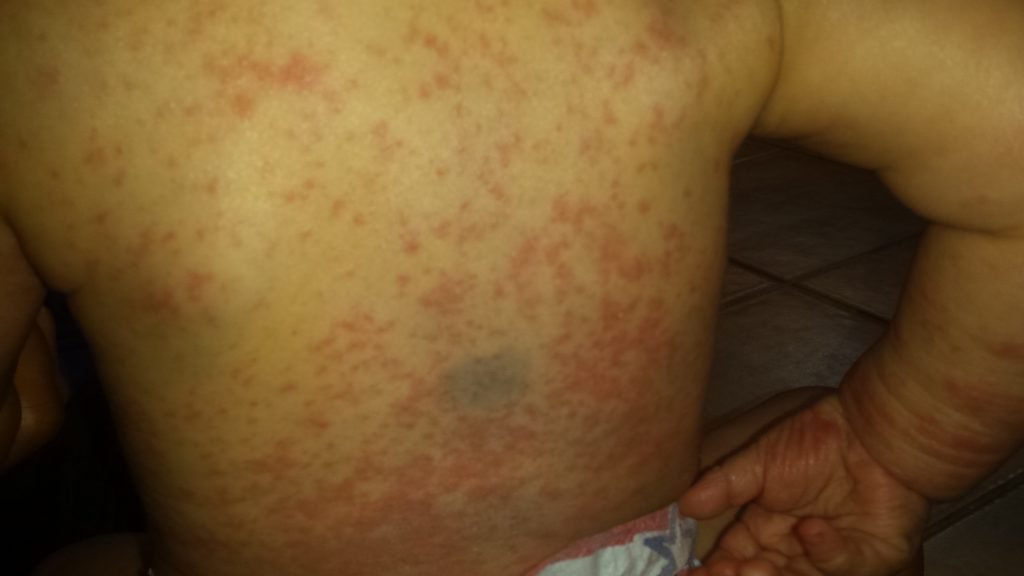
Figure 1. Before Treatment
Assessment & Plan
The patient had significant family medical history, suggesting a genetic or miasmatic predisposition to eczema. Rice cereal was introduced at 6 months of age. This may have contributed to grain sensitivity and gastrointestinal dysfunction. The patient’s diet included several potential allergens, including gluten, cheese, oats, and tomatoes. We started by running a bloodspot IgG food antibody test.
I prescribed an elimination diet, as well as assorted products to support gastrointestinal health and promote detoxification, including a nutritional formula for intestinal healing (containing various sulfhydryl compounds and D-ribose), a probiotic, and an herbal hepatic detox formula. I prescribed liquid zinc and a liquid vitamin/mineral formula to account for gastrointestinal malabsorption. I also suggested an OTC petroleum jelly alternative (containing soy oil, beeswax, vitamin E, and rosemary oils) and homeopathic Argentum metallicum – 2 topical ointments to support skin hydration, decrease infection, and promote skin healing. At this visit, I felt that the patient’s homeopathic evaluation indicated a Pulsatilla symptom picture. One dose was administered at the visit. The patient’s skin appeared to slightly decrease in inflammation after the dose.
Follow-Up Between Visits
After 2 days of Pulsatilla 30C dosing, the patient’s mother reported that David’s appetite had increased, his skin was slightly less irritated and erythematous, and he was less fussy. After 10 days, she reported that he was improving little by little every day. I instructed the patient’s mother to administer another dose of Pulsatilla 30C.
1-Month Follow-Up
The food antibody test revealed multiple high and moderate food sensitivities, and a positive Candida screen. The patient’s sleep, mood, and appetite had improved significantly, but his eczema was only slightly improved.
At this visit, the patient’s eczematous patches looked slightly different. Erythema was slightly decreased, and it looked like many patches were drying out. There were crusty, herpetic eruptions all over his scalp. Some eruptions were still oozing and bleeding, and some were dry and flakey. I repertorized the patient’s symptoms, considered the Psora miasm, and decided to prescribe Psorinum. I administered a dose of Psorinum 30C at the visit.
Follow-Up Between Visits
The day after the Psorinum 30C dosing, the patient’s mother reported that David was acting more “like his old self” (playing, eating with his own hands, etc). She said that his itching and redness had decreased. She later reported that the improvement seemed to wear off after about 6-7 days. I advised her to administer a weekly dose, every Friday evening.
2-Month Follow-Up
The patient’s eczema was 90% improved! He continued to have 2 eczematous spots on his torso, light eczema on his face, and improving patches on his feet. Other than these areas, his . His mood and demeanor had improved significantly. His mother reported that his stools looked more digested.
3-Month Follow-Up
The patient’s eczema continued to improve. His symptoms were about 95% improved from his first visit (Figure 2). The patient’s mother noticed that David’s eczema symptoms would start to increase about 10 days after the Psorinum 30C dosing. She started introducing foods 1 at a time to expand the foods in his diet, and it went well. I advised her to continue the supportive supplements, dose the Psorinum 30C every 7-9 days, and follow up in 1-2 months.
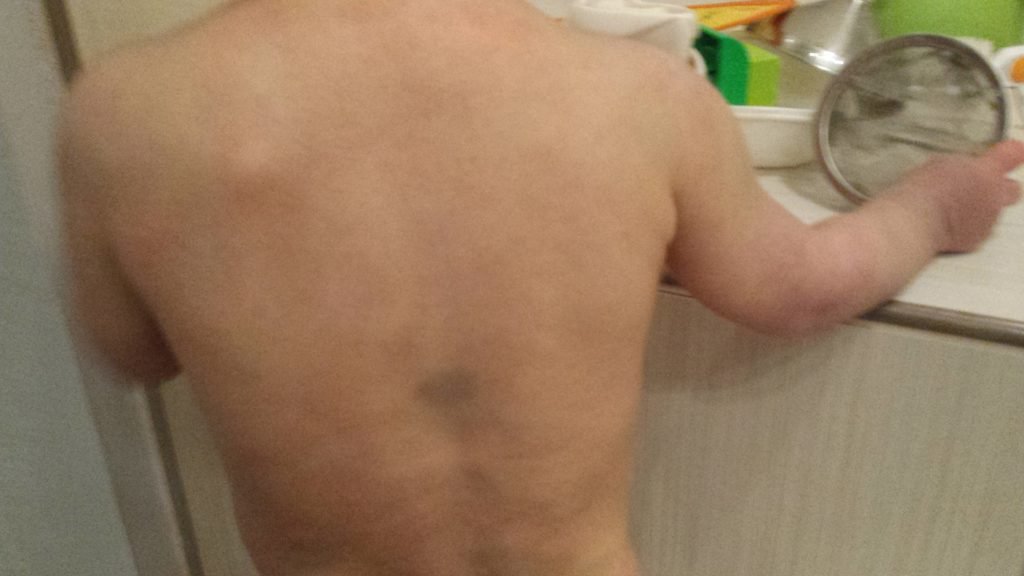
Figure 2. After Treatment
Case Study 2
Kendall, a 2.5-year-old male, presented to my clinic in May 2014 with severe atopic dermatitis, Hand Foot and Mouth Disease (HFMD), a chronic cough, and congestion. The patient was diagnosed with HFMD on April 7, 2014; at the first visit he continued to have open sores on his feet and hands, along with severe eczema on his ears, back, arms, abdomen, neck, feet, and thighs.
First Visit
History
The patient had eczema since birth, but his eczema flared most severely after contracting HFMD. The patient had jaundice at birth. They ran a food allergy panel, and all foods were negative. They have maintained a relatively allergen-free diet, with the exception of cow’s milk, yogurt, and eggs. The patient is still breastfeeding twice daily. Kendall’s mother, father, and grandparents all have eczema.
Homeopathic
The patient’s mother describes Kendall’s personality as emotional, intense, irritable, vocal, excitable, playful, decisive, good sense of humor, and easily bored. At the office, I observe him to be curious, robust, and extroverted. He craves sweet fruits and foods, apple, breads, and meat. His body temperature is hot, and he sleeps with 1 foot sticking out from under the covers. His symptoms are worse with heat, and he overheats easily. He thrives when he is the center of attention.
Objective
The patient is drooling excessively. He has erythematous patches on back, abdomen, arms, neck, feet, itchy thighs, and behind his ears. Postauricular patches are weeping and crusting over, and the patches on his neck have yellow crusts.
Assessment & Plan
The patient had significant family medical history, suggesting a genetic or miasmatic predisposition to eczema. The patient’s diet included some potential allergens, including cow’s milk and eggs. We started by running a 96-food IgG panel. The patient was already doing a modified elimination diet, so I instructed his mother to try the Blood Type B diet until the food sensitivity results came in.
I prescribed a probiotic and nutritional formula for intestinal healing (containing various sulfhydryl compounds and D-ribose) to support gastrointestinal health, and liquid zinc, fish oil with vitamin D, and a liquid multivitamin to account for malabsorption of nutrients. To soothe and heal his skin, I prescribed a soothing cream containing Calendula, neem, and probiotics. The patient’s homeopathic evaluation indicated a Sulphur symptom picture. Sulphur is a well-known Psoric remedy. The patient’s mother was instructed to administer 1 dose of Sulphur 6C daily.
1-Month Follow-Up
The patient had stopped drooling. The eczema on his abdomen, postauricular area, and legs was improved. The eczema on his hands, behind his neck, and back had worsened or stayed the same. Labs revealed multiple food sensitivities. The patient’s mother was instructed to continue the treatment plan and avoid all food sensitivities until the next visit.
2-Month Follow-Up
Sleep had improved. The patient was no longer waking up 4 times per night. The patient was less congested and his stool had improved. His skin had improved, but the improvement was plateauing. I decided to increase the potency of Sulphur to 30C, only 1 dose, and then follow up in 2 weeks.
2.5-Month Follow-Up
The patient’s mother reported that Kendall’s sleep had improved by “leaps and bounds” on the Sulphur 30C. His mood and skin had improved significantly. I instructed her to continue dosing Sulphur every 2 weeks until the next visit.
3.5-Month Follow-Up
All eczematous patches were much improved. The patches were only limited to hands, postauricular areas, and folds of legs and arms, and they were less inflamed, dry, and erythematous. Torso, back, neck, and face were clear of patches. The patient was happy and cooperative at the visit. I instructed the patient’s mother to discontinue zinc and to continue all other supplements and biweekly dosing of Sulphur 30C.
4.5-Month Follow-Up
Eczematous patches on neck, dorsal feet, dorsal hands, and postauricular areas had improved significantly. The only remaining area with eczematous patches was the postauricular area, but they were much improved since the last visit. I instructed the patient’s mother to discontinue the intestinal healing formula and to continue the children’s multi, the probiotic, vitamin D, fish oil, Cal/Mag, and biweekly dosing of Sulphur 30C.
Discussion
In both cases, the patient’s parents reported that changing the diet (ie, clearing the obstacle to cure) resulted in the most improvement, followed by the dosing of the homeopathic remedy (ie, clearing the Psora miasm). If I had prescribed the remedy without changing the patient’s diet, it is possible that the healing would not have been as quick or as complete. Hahnemann says in the Organon of Medicine, “[If] the best selected homoeopathic (antipsoric) medicine in the suitable (minutest) dose does not effect an improvement… there is some circumstances in the mode of life of the patient or in the situation in which he is placed, that must be removed in order that a permanent cure may ensue.”2 Before a well-chosen remedy can stimulate the body’s self-healing ability, or the “Vis,” the “obstacles to cure”2 must be addressed. I believe that this is the key to success in treating a child with eczema.
In the first case, I first prescribed the remedy Pulsatilla, based on the patient’s symptom picture and personality, without taking the Psora miasm into consideration. At the following visit, after the Pulsatilla, diet, and supportive supplements had cleared some obstacles and improved the patient’s sleep, mood, and appetite, I was able to see the Psora miasm more clearly. Once the patient was given Psorinum 30C, he improved drastically. The patient’s mother is very happy with his progress and I will be following up with them in a couple of weeks.
In the second case, I saw the Psoric picture more clearly and I started with the Sulphur 6C remedy. After increasing to the 30C potency, the patient’s symptoms improved tremendously. I recently contacted the patient’s mother, and she reports that he is symptom-free. He maintains an allergen-free diet and takes a multivitamin, but he no longer needs to take the Sulphur 30C.
In a pediatric atopic dermatitis case, as we have seen here, the Psora miasm is almost always present. A well-prescribed Psoric remedy given at an early age can clear the miasm, strengthen the Vis, and set the patient up for a lifetime of optimal health.
Please note: The patient’s name in Case #1 has been changed, as his mother requested that he remain anonymous.
 Diane Angela Fong, ND, is the founder of NaturalStart Naturopathic Family Medicine, in Los Altos, CA. Dr Fong attended the University of Bridgeport College of Naturopathic Medicine after receiving her undergraduate degree in molecular cell biology at UC Berkeley. She believes that a healthy start in life leads to a healthy future, and that chronic disease, especially in childhood, can lead to more serious problems down the line. Because of this, Dr Fong’s practice focuses on treating children and families, and educating them about preventive care. Her special interests include chronic pediatric and adult conditions, chronic skin disease, gastrointestinal complaints, infertility, anxiety, depression, and endocrine-related issues.
Diane Angela Fong, ND, is the founder of NaturalStart Naturopathic Family Medicine, in Los Altos, CA. Dr Fong attended the University of Bridgeport College of Naturopathic Medicine after receiving her undergraduate degree in molecular cell biology at UC Berkeley. She believes that a healthy start in life leads to a healthy future, and that chronic disease, especially in childhood, can lead to more serious problems down the line. Because of this, Dr Fong’s practice focuses on treating children and families, and educating them about preventive care. Her special interests include chronic pediatric and adult conditions, chronic skin disease, gastrointestinal complaints, infertility, anxiety, depression, and endocrine-related issues.
References
- Hahnemann S. The Chronic diseases: Their Peculiar Nature and Their Homoeopathic Cure. Philadelphia, PA: Boericke & Tafel; 1904.
- Hahnemann S, Boericke W. Organon of Medicine. Philadelphia, PA: Boericke & Tafel; 1901.