Tolle Causam
Donna Beck, ND
Once you start noticing it, you see it everywhere: the pink scum that accumulates at the edges of your bathtub, in the kitty’s water bowl, in the crevices of your sink, and even in the water holder compartment of your coffeemaker.
You wonder what is this? Then you begin to see it by its scientific name, Rhodotorula, an abnormal finding in the laboratory results of your patient’s gastrointestinal (GI) panel. The “pink” has somehow manifested itself inside your patient! Could this organism be the source, in whole or in part, of your patient’s complaints? Then, you recall that you have actually seen this organism on quite a few GI panels for other patients as well, but you did not think much about it at the time. It was just another pesky, opportunistic fungus, after all.
As it turns out, this valentine pink fungus is the Rhodotorula genus. And it is no wimp.
“Pinkie” may be the new tough chick in town, and she appears to be here to stay. Previously considered a nonpathogenic organism, she has been recognized for the past 2 decades as an emerging yeast pathogen in humans.1 Research reveals numerous articles beginning with statements like “Rhodotorula species have been increasingly recognized as emerging pathogens, particularly in immunocompromised patients.”2 It seems that Pinkie is rapidly gaining ground as a potential “mean girl” gang member as far as unfriendly colonies go in the gut ecological system.
The genus Rhodotorula includes 8 species, of which Rhodotorula mucilaginosa, Rhodotorula glutinis, and Rhodotorula minuta are known to cause disease in animals and humans.2 Rhodotorula is now the most common microorganism isolated from swabs of hospital employees’ and patients’ hands; R mucilaginosa is the most common species, followed by R glutinis and R minuta.3
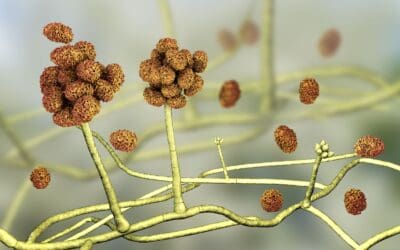
Rhodotorula species are ubiquitous saprophytic yeasts, which live off dead or decaying matter. Rhodotorula species produce pink to red colonies and blastoconidia (budding cells) that are unicellular, lacking pseudohyphae and hyphae.
The resilience of this organism can be seen in its affinity for a wide variety of environments. Rhodotorula has been isolated in some of the most inhospitable ecosystems and environments on earth.
Several authors describe the isolation of this fungus from sites with unfavorable conditions, including the depths of the Baltic Sea, the high-altitude Lake Patagonia, the soil and vegetation of Antarctica, and aquatic, hypersaline, and high-temperature environments such as the Dead Sea in Israel, Lake Enriquillo in the Dominican Republic, the Great Salt Lake in the United States, and beaches located in northern Brazil.4-7 In one study,7
R mucilaginosa was the third most isolated yeast in seawater. Another study8 reported the occurrence of Rhodotorula species in marine waters polluted by household waste.
Rhodotorula Has a Strong Affinity for Plastic and Fruit
Our not-so-friendly, pink fungus has been isolated from various types of medical equipment such as dialysis equipment, fiber-optic bronchoscopes, and venous catheters. It has been cultured from many everyday items made of plastic, including shower curtains, bathtubs, and toothbrushes.9 Rhodotorula mucilaginosa is one of the most common organisms found on athletic mouth guards; because of this, athletes who wear protective mouth guards and individuals who wear dental appliances are advised to rinse these appliances daily with antifungal solutions.10 One study11 recommended that music teachers should be aware that woodwind and other musical instruments with plastic mouthpieces could be a source of Rhodotorula fungus and other pathogenic microorganisms. Commercially prepared fruit salads from grocery store coolers, pasteurized fruit juices, and soy milk were found with high concentrations of Rhodotorula and other fungal organisms.12 Quite surprising is the research that cautions immune-compromised individuals against consuming coconut water products as they were found to contain Rhodotorula and other resistant fungal species that could lead to fungemia.13
Rhodotorula in a Case of Epilepsy
Three years ago, I ordered an expanded GI panel on an 11-year-old girl who presented with constipation and intermittent bouts of abdominal pain and loss of appetite. I was surprised when her results came back with +3 Rhodotorula (on a scale of +1 to +5, with 0 indicating normal) but no other pathogens whatsoever. I had fully expected abnormal bacteria, imbalanced flora, or perhaps even parasites, based on her history and physical examination findings. If fungus was in her intestinal tract, I thought it would be the ever-so-common Candida species.
The intestinal secretory IgA level on her GI report was more than 1350 mg per 100 g (dry weight) of stool (with normal being 400-800 mg per 100 g). These results indicated that her intestinal immunity, the body’s first line of defense, was fiercely activated. Many articles relating to intestinal candidiasis and elevated intestinal secretory IgA were available, but I found very little information at that time regarding Rhodotorula.
Her alpha anti-chymotrypsin stool level was 98 mg per 100 g (dry weight) (with normal being <60 mg per 100 g), indicating borderline colitis. This patient also had a low output of pancreatic enzymes as indicated by a chymotrypsin level of less than 3 U per 10 mg (with normal being >9 U per 10 mg). I found this unusual in an otherwise healthy child.
Since I considered fungus as opportunistic, I began focusing on potential allergens, especially gluten sensitivity, as a cause for lowered immune resistance that would allow the yeast to invade in the first place. Even though her test results for gluten sensitivity were normal, I focused on this area because it is so often the culprit, but this approach did not help her.
Within a year of the initial evaluation, this young girl began to have seizures and was diagnosed as having epilepsy without known cause and was started on anticonvulsant medications by a neurologist. At this point, her constipation was decidedly chronic, as were her nausea, sensitive appetite, and intermittent abdominal cramps. She had signs of evolving leaky gut syndrome in spite of my numerous naturopathic interventions to specifically prevent this.
In naturopathy, we postulate that leaky gut can allow neurotoxic substances to enter the bloodstream. As leaky gut worsens, so does neuronal toxicity. This patient is now 14 years old and has continued to have cyclical bouts of intestinal distress and allergy reactions. She has required a much stronger anticonvulsant medication regimen. Could the Rhodotorula have been the cause of her increasing leaky gut symptoms? Was it more pathogenic than I had initially considered? It was this case and the fact that I began to see other patients with similar GI panel results that motivated me to research Rhodotorula. Recently, her parents wholeheartedly agreed to another functional GI panel test for her. I am eager to assess if the Rhodotorula is still present in her intestinal tract.
Rhodotorula After Scoping the Colon
A female patient in her early 50s had very few intestinal complaints until she underwent a routine colonoscopy. Her colonoscopy was normal except for mild diverticula, but since that procedure she had experienced months of unrelenting diarrhea. We tried many things to alleviate it, including probiotics, a careful diet, colonic therapy, and even a therapeutic course of fluconazole in case she had developed Candida enteritis. Nothing was helping, so I ordered a comprehensive GI panel to see if she had abnormal organisms in her GI tract.
The results showed that she had plenty of normal flora and no other pathogens except for +2 Rhodotorula. Her intestinal secretory IgA findings were in the inflammatory range at greater than 1370 mg per 100 g (dry weight) of stool. These findings again showed fierce activation of gut immune defense. Her alpha anti-chymotrypsin stool level was 121 mg per 100 g (dry weight), indicating moderate colitis. Her chymotrypsin level was 8 U per 10 mg, indicating mildly low pancreatic enzyme production.
I learned that Rhodotorula is reliably resistant to fluconazole and echinocandins but is generally susceptible to amphotericin B and flucytosine.14 After treating the patient with compounded capsules of amphotericin B (100 mg BID orally) for 10 days, she began to improve, but not completely. Since adding gut restoration substances (which included glutamine and digestive enzymes) and strictly avoiding her allergens, she has steadily improved.
I also counseled the patient to avoid fruit juices and coconut water, which she had been using in large amounts to replenish the electrolytes lost from diarrhea. I asked her to avoid storing food in plastic containers. I suggested that she use a water filter on her sink instead of water from standing units where water sits in plastic all day. She was to rinse all fruit with an antifungal solution and chop fruits and vegetables at the time of consumption rather than letting them stand for any length of time. She was also instructed to buy a new toothbrush each month and rinse it daily in hydrogen peroxide solution. Finally, she had to clean her sink and bathtub just before each use. Repeat testing at 3 months showed that Rhodotorula had left her system.
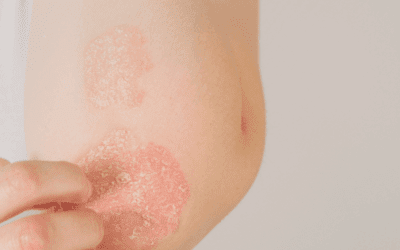
Rhodotorula in a Healthy Cancer Survivor With Eczema
A woman in her early 50s had a history of uterine cancer that had been successfully treated. She complained of stubborn chronic eczema that flared with stress and almost constant stomach distress and food reactions. She also felt generally unwell and was motivated to maintain a strong immune system as prevention against further cancer episodes.
Her comprehensive functional GI analysis showed a moderate amount of alpha hemolytic Streptococcus, a rare amount of Klebsiella pneumoniae, but a large amount of Rhodotorula species at +3. This patient had a secretory IgA level that was quite suppressed; hers was 16 mg per 100 g (dry weight) of stool. Her chymotrypsin level was low normal at 8 U per 10 g, indicating low pancreatic enzyme output. Her alpha anti-chymotrypsin stool level was 48 mg per 100 g (dry weight), which was in the normal range. No colitis was present. This patient also had a low serum white blood cell count.
These values were low in the face of infection. Her immune system did not seem to be challenging the fungus, as I had seen in other patients. I began treatment with compounded amphotericin B (100 mg BID orally) for 10 days, along with a comprehensive diet supplement and herbal medicine program. At 6 months, all of her complaints were either eliminated or very mild. No yeast were isolated on repeat testing. Her intestinal secretory IgA level had risen to 49 mg per 100 g (dry weight) of stool. This level was still not normal, but it was an improvement. Her chymotrypsin level was now normal at 9 U per 10 g, indicating improved and normalized pancreatic enzyme production. Unfortunately, her alpha
anti-chymotrypsin stool level was not retested, but the other distinct positive was that her serum white blood cell count was now well within the normal range.
Conclusion
Wirth and Goldani alert us to be on the lookout for more news regarding this fungal pathogen: “Further studies are needed to clarify the role of food contamination by Rhodotorula and the development of opportunistic fungal infections.”15 Evidence suggests that Rhodotorula can not only affect individuals who are already immune compromised but also can colonize in the human digestive tract and become a source of chronic infection in otherwise healthy individuals, causing a battle between fungus and gut defense mechanisms. Wirth and Goldani further state:
“These future studies should focus on the survival and growth of Rhodotorula in the gastrointestinal system and its potential ability to transfer from the gastrointestinal tract to bloodstream and should seek to better understand the ecology of Rhodotorula in hospitals and healthcare environments.”15
In the sporting of her colors, Pinkie actually should be the red flag for healthier choices as she shows us yet another reason to consider using less plastic in our everyday lives, especially when it comes in contact with our food and beverages and our bodies. We see 1 more reason to use freshly prepared foods vs those that are offered to us through industrialization. And we are again reminded of the long-standing naturopathic admonition to keep the gut defenses strong.
 Donna Beck, ND graduated from the National College of Natural Medicine (Portland, Oregon) in 1992, after which she completed a 2-year family residency at NCNM’s teaching clinic. Dr Beck has maintained a private practice (A Family Wellness Center) for the past 20 years in Portland. As a primary care physician and expert in natural medicine, Dr Beck sees people of all ages and treats most common conditions. Dr Beck taught students of natural medicine for more than 15 years at NCNM, serving as an attending physician at the teaching clinic there. She served for 3 years on the board of directors at NCNM, as well as on the Oregon Board of Naturopathic Medicine. Dr Beck is a current member of the Oregon Association of Naturopathic Medicine and the American Association of Naturopathic Medicine.
Donna Beck, ND graduated from the National College of Natural Medicine (Portland, Oregon) in 1992, after which she completed a 2-year family residency at NCNM’s teaching clinic. Dr Beck has maintained a private practice (A Family Wellness Center) for the past 20 years in Portland. As a primary care physician and expert in natural medicine, Dr Beck sees people of all ages and treats most common conditions. Dr Beck taught students of natural medicine for more than 15 years at NCNM, serving as an attending physician at the teaching clinic there. She served for 3 years on the board of directors at NCNM, as well as on the Oregon Board of Naturopathic Medicine. Dr Beck is a current member of the Oregon Association of Naturopathic Medicine and the American Association of Naturopathic Medicine.
References
Louria DB, Greenberg SM, Molander DW. Fungemia caused by certain nonpathogenic strains of the family Cryptococcaceae. N Engl J Med. 1960;263:1281-1284.
Tuon FF, Costa SF. Rhodotorula infection: a systematic review of 128 cases from literature. Rev Iberoam Micol. 2008;25(3):135-140.
Strausbaugh LJ, Sewell DL, Tjoelker, RC, et al. Comparison of three methods for recovery of yeasts from hands of health-care workers. J Clin Microbiol. 1996;34(2):471-473.
Ekendahl S, O’Neill AH, Thomsson E, Pedersen K. Characterisation of yeasts isolated from deep igneous rock aquifers of the Fennoscandian Shield. Microb Ecol. 2003;46(4):416-428.
Libkind D, Brizzio S, Van Broock M. Rhodotorula mucilaginosa, a carotenoid producing yeast strain from a Patagonian high-altitude lake. Folia Microbiol (Praha). 2004;49(1):19-25.
Pavlova K, Grigorova D, Hristozova T, Angelov A. Yeast strains from Livingston Island, Antarctica. Folia Microbiol (Praha). 2001;46(5):397-401.
Butinar L, Santos S, Spencer-Martins I, et al. Yeast diversity in hypersaline habitats. FEMS Microbiol Lett. 2005;244(2):229-234.
Hagler AN, Mendonca-Hagler LC. Yeasts from marine and estuarine waters with different levels of pollution in the state of Rio de Janeiro, Brazil. Appl Environ Microbiol. 1981;41(1):173-178.
Querol A, Fleet GH, eds. Yeasts in Food and Beverages (The Yeast Handbook). Berlin and Heidelberg, Germany: Springer; 2006, p. 381.
Glass RT, Conrad RS, Köhler GA, et al. Microbiota found in protective athletic mouth guards. Sports Health. 2011;3(3):244-248.
Glass RT, Conrad RS, Kohler GA, Bullard JW. Evaluation of the microbial flora found in woodwind and brass instruments and their potential to transmit diseases. Gen Dent. 2011;59(2):100-107.
Toumas VH, Heeres J, Burgess L. Molds and yeasts in fruit salads and fruit juices. Food Microbiol. 2006;23(7):684-688.
Maciel NO, Piló FB, Freitas LF, et al. The diversity and antifungal susceptibility of the yeasts isolated from coconut water and reconstituted fruit juices in Brazil.
Int J Food Microbiol. 2013;160(3):201-205.
Nunes JM, Bizerra FC, Ferreira RC, Colombo AL. Molecular identification, antifungal susceptibility profile, and biofilm formation of clinical and environmental Rhodotorula species isolates. Antimicrob Agents Chemother. 2013;57(1):382-389.
Wirth F, Goldani LZ. Epidemiology of Rhodotorula: an emerging pathogen. Interdiscip Perspect Infect Dis. 2012;2012:465717. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3469092/. Accessed February 17, 2013.