Sportin’ Life
Conventional and CAM Treatments for Osgood-Schlatter Disease
Katie Baker, ND, LMP
Osgood-Schlatter (OS) disease is the inflammation of the apophysis (cartilage growth plate) of the tibial tuberosity, caused by excessive use of the quadriceps tendon. It is typically found in athletic children, particularly those aged 12-16 years, although a primary incident can occur at a younger age, especially in females, and in the late teens as well. A 21% incidence in athletes, compared to a 4.5% incidence in the general population of adolescents, strongly defines OS as an overuse condition rather than a normal condition of adolescence.1 We see a higher frequency in males, but this may be due to a higher number participating in sports, in general, compared to females. As we see more adolescent females participating in sports at a more competitive level, we may see the incidence of OS rise in this group.
In a typical OS patient, we see pain and swelling on the proximal portion of the anterior surface of the tibia, with tenderness over the bony prominence (tibial tuberosity) immediately below the knee where the quadriceps tendon inserts laterally (see Figure 1). This knee pain worsens with activity, especially kneeling, jumping, and climbing stairs. It is better with rest and is typically accompanied by tightness in the quadriceps and other surrounding muscles.2
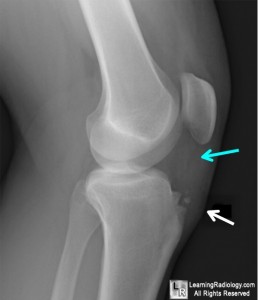
Figure 1
Differential Diagnoses
Other conditions to rule out in the diagnosis of OS include Sinding-Larson-Johansson Syndrome (a similar condition that affects the lower portion of the patella instead of the tibial tuberosity,3 benign or malignant tumors of the bony and soft tissue, chondromalacia patellae, patellar tendonitis, quadriceps tendon avulsion, osteomyelitis of the tibia, synovial plica injury (irritation of the synovial capsule), fracture of the tibial tuberosity, infectious apophysitis, or accessory ossification centers. Two additional conditions on the list of differential diagnoses include: Perthes disease, which affects the hip joint but has pain that can radiate to the knee; and Hoffa’s syndrome, involving the fat pad below the patella.1
Conventional Treatment of Osgood-Schlatter
Conventional treatment of OS is very conservative, typically relying on the RICE protocol (Rest, Ice, Compression, and Elevation), NSAID use as needed, and some physical therapy. As most children diagnosed with OS are competing at more serious athletic levels, the Rest component of RICE may be modified so that the athlete should avoid unnecessary drills rather than being completely inactive or unable to compete. Braces may be used for immobilization and compression. Physical therapy includes direct work on strengthening and stretching the muscles of the thigh, with particular attention to loosening the quadriceps muscles. Instructional videos can be found online to assist in parent and patient education for these stretches and strengthening exercises.4,5
In cases of OS that are resistant to conservative treatments, studies have been done reviewing the efficacy of surgical interventions. Surgical interventions for removal of osseous fragments have a particularly high success rate.6,7 These procedures should be considered as an option if separate fragments are visualized through imaging and both conservative and CAM treatments are not successful. One study of young men in the military showed that 87% had no restrictions in daily activity 10 years post-surgery and 75% had returned to their pre-operative level of sports activity.6 A small study in Israel (n=22), using local anesthetic to remove ossicles on the tibial tuberosity, showed that all subjects had returned to their full exercise routine after 12 weeks, with only one reporting pain upon kneeling.7
Extracorporeal shock wave therapy is another form of conventional treatment that is gaining favor in the treatment of OS. While recent studies supporting this therapy can be found in PubMed,8 its use is contraindicated with open bone growth plates, leading one to wonder if this would be a viable therapy for adolescents, still undergoing growth, or if it would be better reserved for adults suffering from sequelae or recurrence of OS.
Alternative Medicine Treatments for Osgood-Schlatter
CAM treatments for OS, and for physical injuries and ailments, in general, do an excellent job of supporting traditional treatments and providing pain relief and, in many cases, providing symptomatic improvement for conditions that conventional medicine treats with a conservative approach.
In the physical medicine modality, ultrasound and iontophoresis (delivery of medicines transcutaneously via ultrasound), sports-taping, and the hands-on therapies can help. Using the Graston technique, a form of fascial restriction release using a metal implement, on the quadriceps muscles can help to reduce muscle tightness and adhesions that contribute to OS symptoms.9
In England, a physiotherapist named Jenny Strickland (no affiliation) has created a stretching and massage protocol to be implemented by parents at home that claims a return to full activity in 3 weeks. Their small clinical study (n=25) measured tendon load to pain onset (using a standing wall squat test). Treatment included a myofascial release massage period until pain-free knee flexion was achieved, followed by a period of quadriceps stretching. At the completion of the study (50 days), all of the child athlete subjects achieved a full, pain-free wall squat (mean length of time, 20 days).10
Muscle relaxation is an important component to relieving the pain of OS. To this end, topical castor oil, calcium and magnesium supplements, and Epsom salt baths can be of benefit to our OS patients. Acupuncture, long used for pain relief, is another potentially beneficial treatment modality. Acupuncture has been shown to increase microcirculation, to aid in dispersal of swelling, to suppress inflammation and to promote faster recovery after training sessions.11
Prolotherapy, the injection of an irritant into a ligament or tendon to promote the growth of new tissue, also shows promise in the treatment of OS. A 2011 study on subjects with recalcitrant OS, published in Pediatrics, compared monthly dextrose or dextrose/lidocaine injections and standard care in terms of their effects on sports-related symptoms and changes to activity level.12 At 3 months, changes to activity level were less frequent in both the dextrose-treated and lidocaine-treated knees, and changes to sports-related symptoms were decreased in dextrose-treated knees. After 1 year, the study found that athletes treated with dextrose injections were less symptomatic in both areas than the athletes given either the dextrose-lidocaine injections or standard care.
Nutritional support via antioxidant therapy can assist inflammation reduction in OS as well. Selenium and vitamin E show great promise in this area. The dosage is 200 mcg of selenium and 400 IU of vitamin E for 1-2 months, followed by 50-100 mcg of selenium daily.13 More than 20 years of positive anecdotal evidence indicates that this protocol would be an interesting area of more formalized study.
Conclusion
In conclusion, Osgood-Schlatter disease occurs in as many as 20% of child athletes and can recur later in life. Currently, more boys than girls suffer from it, but that number may reflect differences in athletic activity between genders. While prevention of symptom-aggravating activity may not be possible, there are a number of effective treatments available that don’t require surgery or pharmaceutical interventions.
NDs with a focus on physical medicine or pediatrics will need to enlist parent aid in order to achieve the best resolution to this ailment. Expecting a child or teen to avoid playing a sport that they love in addition to completing sports rehabilitation is unrealistic. However, many student athletes have parents who are deeply involved in their child’s activities. The “stage mother” in sports may be a singular challenge that, if approached in the proper way, can improve outcomes rather than hindering them. Re-routing the overly-engaged parent’s focus from competition to successful completion of in-home treatments and rehabilitative routines will ensure patient compliance with prescribed treatments, activity reduction, and a return to the playing field or court sooner and in the best possible condition.
 Katie Baker, ND, LMP is a naturopathic physician, licensed massage therapist, and owner of Stone Turtle Health in Ballard, WA. She has over 20 years of experience working with children and families. As a family practitioner, Dr Baker works to make naturopathic medicine accessible to every family in her community. Her passions include volunteering (especially with the Make-A-Wish Foundation), sailing, quilting, improvisational comedy, and spending time with her own family.
Katie Baker, ND, LMP is a naturopathic physician, licensed massage therapist, and owner of Stone Turtle Health in Ballard, WA. She has over 20 years of experience working with children and families. As a family practitioner, Dr Baker works to make naturopathic medicine accessible to every family in her community. Her passions include volunteering (especially with the Make-A-Wish Foundation), sailing, quilting, improvisational comedy, and spending time with her own family.
References
- Sullivan JA, Young CC Chang AK, et al. DeBerardino. Osgood-Schlatter Disease. Updated February 20, 2013. Medscape Reference. http://emedicine.medscape.com/article/1993268-overview. Accessed March 28, 2013.
- Mayo Clinic staff. Osgood-Schlatter disease. Mayo Clinic Web site. http://www.mayoclinic.com/health/osgood-schlatter-disease/DS00392/DSECTION=symptoms. Accessed March 28, 2013.
- Osgood-Schlatter, Sinding-Larsen-Johansson, and Sever Syndromes. In: Kid’s Sports Corner newsletter. May, 2010. Children’s Orthopaedics of Atlanta Web site. http://www.childrensortho.com/kids-sports-corner-osd.html. Accessed March 28, 2013.
- Sports Injury Clinic. Osgood Schlatters Disease. Sports Injury Clinic Web site. http://www.sportsinjuryclinic.net/sport-injuries/knee-pain/osgood-schlatters-disease. Accessed March 28, 2013.
- Durkin T. Osgood-Schlatter’s Disease – Athletic Edge. October 20, 2009. YouTube Web site. http://www.youtube.com/watch?v=Yh6YekgJygs. Accessed March 28, 2013.
- Pihlajamäki HK, Visuri TI. Long-term outcome after surgical treatment of unresolved Osgood-Schlatter Disease in young men: surgical technique. J Bone Joint Surg Am. 2010;92 Suppl 1 Pt 2:258-264.
- Nierenberg G, Falah M, Keren Y, Eidelman M. Surgical treatment of residual Osgood-Schlatter Disease in young adults: the role of the mobile osseous fragment. Orthopedics. 2011;34(3):176.
- Lohrer H, Nauck T, Scholl J, et al. Extracorporeal shock wave therapy for patients suffering from recalcitrant Osgood-Schlatter disease. Sportverletz Sportschaden. 2012;26(4):218-222.
- Wilhelm J. Graston Technique Knee Injury. June 7, 2012. YouTube Web site. http://www.youtube.com/watch?v=CGeM-DuDmo4. Accessed March 28, 2013.
- Strickland JM, Coleman NJ, Brunswic M, Kocken R. Osgood Schlatter’s Disease: The Strickland Protocol. June, 2008. http://www.osgood-schlatter-disease.com/osgood-schlatter-clinical-trials.html. Accessed March 28, 2013.
- Acupuncture for Osgood-Schlatter’s Disease. The Sean Barkes Clinic. http://www.theseanbarkesclinic.co.uk/pages/problems-we-treat/painful-conditions/osgood-schlatters-disease.html#.UVSUohziguc. Accessed March 28, 2013.
- Topol GA, Podesta LA, Reeves KD, et al. Hyperosmolar dextrose injection for recalcitrant Osgood-Schlatter Disease. Pediatrics. 2011;128(5);e1121-e1128.
- Keller M. Summer Sports Season. May 31, 2011. Radiant Health Natural Medicine. [Blog]. http://www.radiantnaturalhealth.info/summer-sports-season/. Accessed March 30, 2013.