Case Study: Neuroendocrine Imbalance- Assessing and Treating Pediatric OCD
Heidi Hook, ND
John is an 11-year-old boy whose parents brought him to see me for his obsessive-compulsive behavioral symptoms: He had to follow an exact bedtime routine. Everything in his room had to be in a precise place. The blanket and the sheet had to line up perfectly. Anything amiss would lead to increased irritability, agitation and tantrums.
John also had many fears. He could not take a shower by himself with the shower curtain closed; he had a fear of spiders. When working on a difficult project, he would get angry, blow up and stop working on it. Other symptoms included unstable energy (either tired or hyper), morning fatigue, insomnia, dermographia, asthma, post-nasal drip and chronic coryza, mild hypoglycemia, anxiety, depression, nervousness and irritability. His diet consisted of waffles, cereal or soup for breakfast; tortillas, meat, cheese and beans for lunch; snacks of fruit and popsicles; and a lot of juice. Dinner was standard meat; rice, potato or pasta; and a vegetable. John was very quiet on the first visit, yet was willing to take some supplements. Diet changes, I hoped, would come later.
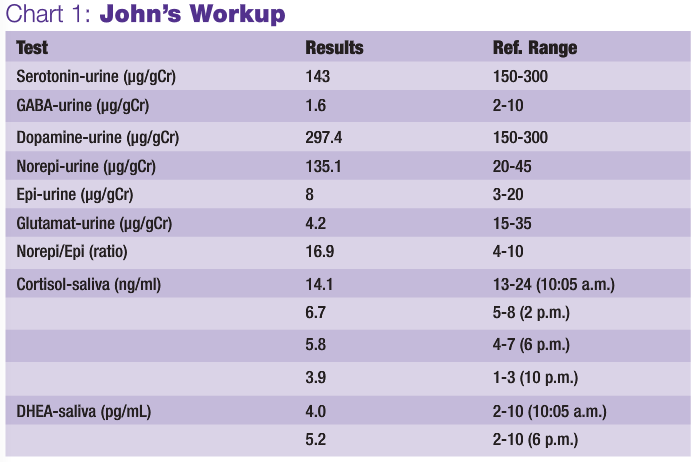
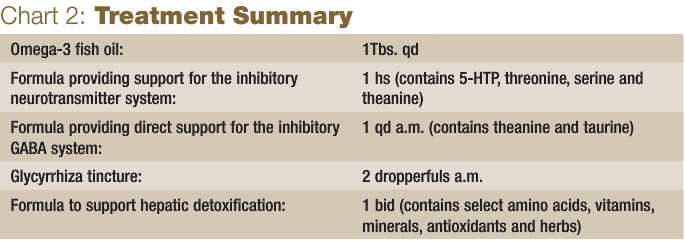
Obsessive-compulsive disorder (OCD) is one of a number of neuroendocrine imbalances. Others include depression, insomnia, anxiety, fatigue, panic disorder, eating disorders, disturbed focus, nervousness, irritability and more. I see neuroendocrine imbalances in patients on a daily basis, and will often test their adrenal gland function and neurotransmitter levels as part of the workup. When I recognized this type of imbalance in John, I tested both. Low serotonin levels are often associated with OCD, and both anxiety and insomnia are also typical symptoms of deficiencies in this neurotransmitter. See Chart 1 for John’s test results, and Chart 2 for his treatment.
Follow-Up Visits
Four weeks later, John came into my office smiling. He was happier, he was sleeping through the night, his energy was stabilizing, his fears were decreasing. In fact, he said he was seeing how many fears he could face in one day (on that day, he had already faced five fears). His asthma symptoms had decreased, along with his post-nasal drip and chronic congestion. His OCD symptoms had decreased, as well. His bedtime routine had relaxed to where the sheet and blanket did not have to line up and items could be in disorder. His ability to remain focused on tasks without getting upset increased. He was able to sleep over at a friend’s house for the first time. He forgot his toothbrush, but it was OK! His mom commented that going to a sleepover would never have happened before, due to his anxiety.
After another month on the same protocol, everything had continued to improve. His OCD symptoms had diminished, almost to nothing. He was sleeping well and waking refreshed. He felt more relaxed all day long. His energy was good, and balanced. He was more understanding, happier and now wanted to socialize more.
 Heidi Hook, ND is a 1996 graduate of Bastyr University. She has a private practice in Auburn, Calif., which centers on helping people suffering with fatigue, depression, anxiety, hormonal imbalance, thyroid imbalance and gut issues.
Heidi Hook, ND is a 1996 graduate of Bastyr University. She has a private practice in Auburn, Calif., which centers on helping people suffering with fatigue, depression, anxiety, hormonal imbalance, thyroid imbalance and gut issues.